Isotope Incorporation Into Co
Zirconium-89 oxalate was obtained from DC AMS Pharma , which was produced via 89Y89Zr reaction with a specific activity of 352.2±26.4 MBq/g of Zr . Zirconium-89 chloride was obtained from 89Zr-oxalate after the heat vaporization of oxalate by the addition of concentrated HCl. During the UiO-67 nMOF synthesis, 148 MBq of 89ZrCl4 was added into a 2-mL reaction mixture while the same reaction condition was maintained for UiO-67. After obtaining the 89Zr-incorporated UiO-67, cobalt embedding, Py-PAA-PEG-Mal functionalization and F3 conjugation was also carried out for in vitro and in vivo evaluation of 89Zr-Co-UiO-67 conjugates.
Also Check: How Is Colorectal Cancer Diagnosed
What Is The Life Expectancy For Triple
In general, about 91% of all women with triple-negative breast cancer are still alive 5 years after diagnosis. If the cancer has spread to the lymph nodes near the breast the 5 year relative survival rate is about 65%. If the cancer has spread to distant places, the 5 year relative survival rate is 12%.
Gene Silencing Of Spag9 Inhibits Cellular Proliferation And Colony Forming Ability Of Mda
Small interfering RNA mediated gene silencing approach was used to selectively knockdown SPAG9 to study its role in cellular proliferation and colony forming ability. Highly aggressive triple-negative basal subtype MDA-MB-231 cells were used for in vitro gene silencing studies. SPAG9 siRNA construct transfected in MDA-MB-231 cells revealed ablation of SPAG9 protein as compared to control siRNA transfected cells as detected in Western blot analysis . However, residual SPAG9 protein expression was also detected in SPAG9 siRNA transfected cells. Subsequently, MDA-MB-231 cells transfected with SPAG9 siRNA revealed significant reduction in cellular growth as compared to control siRNA transfected cells. Cell growth was reduced by 32% post 72h of treatment . Interestingly, colony forming ability was also significantly reduced by for various cell numbers seeded for MDA-MB-231 cells transfected with SPAG9 siRNA but not in cells transfected with control siRNA .2d). These results indicated that siRNA based knockdown of SPAG9 resulted in significant reduction in cellular growth and colony forming ability of triple-negative MDA-MB-231 cells.
Don’t Miss: What Is Hormone Pellet Insertion
Monoclonal Antibodies Targeting Immune Checkpoints In Metastatic Setting
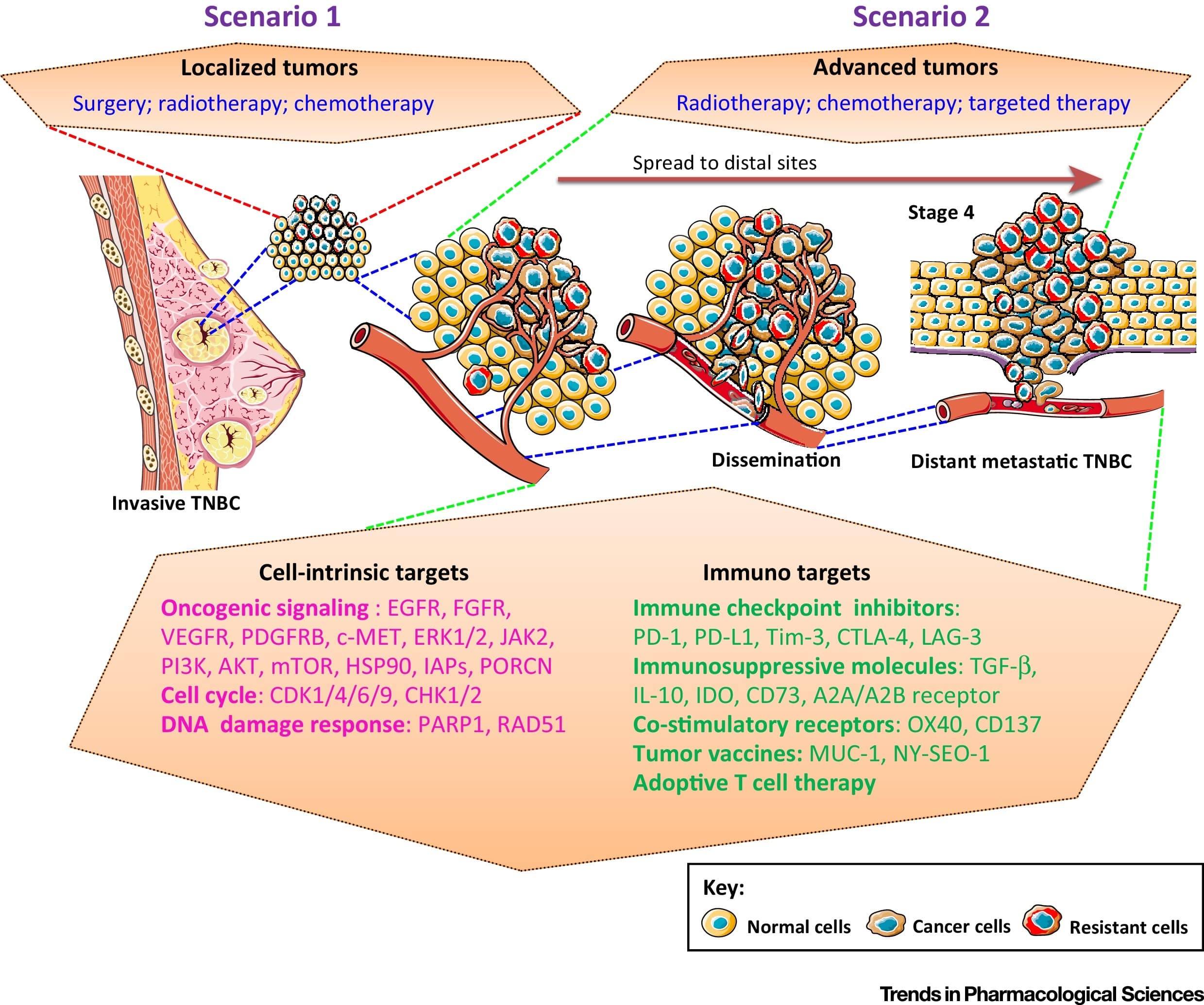
Immune checkpoints are molecules that protect against normal tissue damage caused by over-activity of T-cells . PD-1 and its ligand PD-L1, the most widely studied immune checkpoint receptors in the treatment of breast cancer, are expressed on activated T-cells, B-lymphocytes, and natural killer cells and are associated with tumor immune resistance . An abundancy of genes involved in immune cell processes and high levels of tumor-infiltrating lymphocytes implying high immunogenicity for the IM subtype of TNBC . These characteristics suggest that immune checkpoint inhibitors are feasible therapeutic agents for TNBC. ICIs were first investigated amongst metastatic TNBC patients as a monotherapy. Subsequently, there have been trials to investigate ICIs in combination with chemotherapy agents to enhance response rates, as well as using ICIs in the neoadjuvant setting.
The Prognosis For Patients With Triple
Prognosis refers to the likely outcome of treatment for patients with triple-negative breast cancer. Unlike other types of breast cancer that have a well-proven set of treatments, triple-negative breast cancer is still in the process of being researched for a more standardized treatment plan. Because of this, several treatments may be needed to find one that is effective. Studies have shown that triple-negative breast cancer is more likely to have metastasized , have a higher grade, and are more likely to recur after treatment.
Also Check: How Much Melatonin Should I Be Taking
How Is Triple Negative Breast Cancer Different From Other Types Of Breast Cancer
Triple negative breast cancer is different from other types of breast cancer because it does not have any of the three receptors commonly found on breast cancer cells:
If you have triple negative breast cancer, you may notice that your treatment is slightly different from that offered to other people with breast cancer.
People with oestrogen and/or progesterone receptor positive breast cancer will usually take tamoxifen or an aromatase inhibitor as part of their treatment. People with HER2 positive breast cancer will usually take a drug called Herceptin. These drugs are not effective against triple negative breast cancer.
Recommended Reading: Low Grade Breast Cancer Prognosis
What Is Hormone Therapy
Hormone therapy slows or stops the growth of hormone-sensitive tumors by blocking the bodys ability to produce hormones or by interfering with effects of hormones on breast cancer cells. Tumors that are hormone insensitive do not have hormone receptors and do not respond to hormone therapy.
Hormone therapy for breast cancer should not be confused with menopausal hormone therapy treatment with estrogen alone or in combination with progesterone to help relieve symptoms of menopause. These two types of therapy produce opposite effects: hormone therapy for breast cancer blocks the growth of HR-positive breast cancer, whereas MHT can stimulate the growth of HR-positive breast cancer. For this reason, when a woman taking MHT is diagnosed with HR-positive breast cancer she is usually asked to stop that therapy.
Also Check: Side Effects Hormone Replacement Therapy
Spag9 Mrna Expression In Breast Cancer Cell Lines
RT-PCR analysis revealed that SPAG9 mRNA was found in all breast cancer cell line models used in the present study as shown in Figure 1a. Human testis cDNA was used as positive control which also revealed same size PCR amplicon. Moreover, no expression of SPAG9 transcript was detected in normal mammary epithelial cells which clearly indicated that SPAG9 is expressed exclusively in cancerous cells. Further, PCR amplicon was subcloned in TOPO vector and sequenced. Nucleotide sequencing confirmed the SPAG9 mRNA sequence in all breast cancer cells. Thus, our RT-PCR results indicated that SPAG9 gene is expressed in all breast cancer cells independent of their hormone receptor status or subtypes. We further assessed SPAG9 mRNA expression in normal mammary epithelial cells, MCF7, MDA-MB-231, BT-474 and SK-BR-3 breast cancer cell lines by quantitative real-time PCR. All breast cancer cell lines evaluated displayed higher levels of SPAG9 expression, compared to control normal mammary cells . SPAG9 expression was around 20 fold higher in MCF7, MDA-MB-231 and BT-474. However, 52 fold higher SPAG9 expression was observed in SK-BR-3 as compared to normal mammary cells.
What Is A 5
A relative survival rate compares women with the same type and stage of breast cancer to women in the overall population. For example, if the 5-year relative survival rate for a specific stage of breast cancer is 90%, it means that women who have that cancer are, on average, about 90% as likely as women who dont have that cancer to live for at least 5 years after being diagnosed.
You May Like: How To Balance Cortisol Hormone
Clinical Characteristics Of Tnbc
TNBC is more frequent in younger patients, in BRCA1 mutation carriers, and in specific ethnic groups . TNBC accounts for 39% of breast cancers in African-American women under the age of 50, but only 16% in Caucasian women of the same age group . Histologically, approximately 80-90% of TNBC tumors are invasive ductal carcinomas, with the rest classified as apocrine, lobular, adenoid cystic, medullary, and metaplastic . Besides, TNBCs have increased lymphocytic infiltration, and are high grade with large tumor size. TNBCs are associated with a 4-fold increase in the risk of distant metastases . In contrast to the non-TNBCs which most frequently metastasize to the bone, TNBCs more frequently metastasize to the lungs and the central nervous system . It is estimated that approximately 15-30% of TNBC patients will develop brain metastases . This aggressive metastatic behavior contributes to the overall shortened survival of patients with TNBC compared with non-TNBC. The prognosis of patients with TNBC is very poor, because these tumors are clinically more aggressive than other breast carcinoma subtypes and targeted therapy is ruled out in these patients .
Menopausal Hormone Therapy After Breast Cancer
Taking post-menopausal hormone therapy , also called hormone replacement therapy , to help with menopause symptoms may not be safe for women who have had breast cancer. If you are bothered by menopause symptoms, talk to your doctor about ways to get relief.
Many women have menopause symptoms such as hot flashes after treatment for breast cancer. This can happen naturally as women get older, but it can also be caused by some breast cancer treatments. Some pre-menopausal women have menopause symptoms as a result of chemotherapy or from hormone therapy drugs used to treat breast cancer . Women who are past menopause might also get symptoms if they had to stop taking PHT when they were diagnosed with breast cancer.
Don’t Miss: Kyleena Vs Mirena Hormone Levels
Basal Cell Breast Cancer
Basal cell breast cancer is a type of breast cancer with a clear pattern of changes in proteins in the cells.
Cancer doctors recognise basal cell breast cancer when they examine the cancer cells under a microscope. It is often linked with triple negative breast cancer.
Basal cell breast cancers are usually triple negative. And most triple negative breast cancers are basal cell cancers. They are similar types of breast cancer, but not exactly the same.
See also
The symptoms of triple negative breast cancer are the same as for other breast cancer types.
See also
Moffitt Cancer Centers Approach To Triple Negative Breast Cancer

At Moffitt Cancer Center, we believe in a multispecialty approach to breast cancer diagnosis and treatment. Our Don & Erika Wallace Comprehensive Breast Program comprises highly specialized medical oncologists, radiologists, fellowship-trained surgeons, radiation oncologists and other health care professionals who work together to provide our patients with well-rounded care. Our patients also have access to our supportive care services, which include counseling, integrative medicine, nutritional help and much more.
We continue to make strides in developing our understanding of triple negative breast cancer. Treatments are being evaluated regularly by medical researchers and clinicians as more is being learned about triple negative cancers. Our extensive research efforts and innovative clinical trials help our patients lead healthy and productive lives.
If you are interested in learning more about triple negative breast cancer treatment at Moffitt, call or complete a new patient registration form online.
Recommended Reading: What Is Pellet Hormone Therapy
What Are Hormones And Hormone Receptors
Hormones are substances that function as chemical messengers in the body. They affect the actions of cells and tissues at various locations in the body, often reaching their targets through the bloodstream.
The hormones estrogen and progesterone are produced by the ovaries in premenopausal women and by some other tissues, including fat and skin, in both premenopausal and postmenopausal women and in men. Estrogen promotes the development and maintenance of female sex characteristics and the growth of long bones. Progesterone plays a role in the menstrual cycle and pregnancy.
Estrogen and progesterone also promote the growth of some breast cancers, which are called hormone-sensitive breast cancers. Hormone-sensitive breast cancer cells contain proteins called hormone receptors that become activated when hormones bind to them. The activated receptors cause changes in the expression of specific genes, which can stimulate cell growth.
Breast cancers that lack ERs are called ER negative, and if they lack both ER and PR they may be called HR negative.
Approximately 67%80% of breast cancers in women are ER positive . Approximately 90% of breast cancers in men are ER positive and approximately 80% are PR positive .
How Do Hormone Therapies Work
Hormone therapies slow or stop the growth of hormone receptor-positive tumors by preventing the cancer cells from getting the hormones they need to grow.
They do this in a few ways:
- Some hormone therapies, such as tamoxifen, attach to the receptor in the cancer cell and block estrogen from attaching to the receptor.
- Some hormone therapies, such as aromatase inhibitors and ovarian suppression, lower the level of estrogen in the body so the cancer cells cant get the estrogen they need to grow.
Recommended Reading: What Age Can You Give Child Melatonin
Can Other Drugs Interfere With Hormone Therapy
Certain drugs, including several commonly prescribed antidepressants , inhibit an enzyme called CYP2D6. This enzyme plays a critical role in the body’s use of tamoxifen because CYP2D6 metabolizes, or breaks down, tamoxifen into molecules, or metabolites, that are much more active than tamoxifen itself.
The possibility that SSRIs might, by inhibiting CYP2D6, slow the metabolism of tamoxifen and reduce its effectiveness is a concern given that as many as one-fourth of breast cancer patients experience clinical depression and may be treated with SSRIs. In addition, SSRIs are sometimes used to treat hot flashes caused by hormone therapy.
Many experts suggest that patients who are taking antidepressants along with tamoxifen should discuss treatment options with their doctors, such as switching from an SSRI that is a potent inhibitor of CYP2D6, such as paroxetine hydrochloride , to one that is a weaker inhibitor, such as sertraline or citalopram , or to an antidepressant that does not inhibit CYP2D6, such as venlafaxine . Or doctors may suggest that their postmenopausal patients take an aromatase inhibitor instead of tamoxifen.
Other medications that inhibit CYP2D6 include the following:
- quinidine, which is used to treat abnormal heart rhythms
Molecular Subtypes And Characteristics Of Triple
To avoid blindly developing therapeutic strategies, identifying the complex TNBC subtypes and molecular hallmarks is necessary given that these features are closely linked with clinical outcomes, for example, response to chemotherapy, the pattern of recurrence, and prognosis. Different approaches, including somatic DNA mutation, copy number aberrations, gene expression profiling, and immune metagene information, were applied to analyze TNBCs as a highly diverse group of cancers.
Additionally, molecular alterations were assessed to explore various potential targets for TNBC treatment. It is worth mentioning that a deficiency in homologous recombination, which is partly associated with the loss of breast cancer susceptibility gene function in BC, is correlated with a good response to cisplatin treatment . In an early phase II clinical trial, patients with BRCA-mutant TNBC showed an overall response rate of 80% with single cisplatin therapy . A deficiency in homologous recombination means failure to repair DNA double-strand breaks and damaged DNA replication forks. Therefore, these individuals are also sensitive to poly-adenosine diphosphate -ribose polymerase inhibitors , as PARP is the enzyme that responds to repair DNA single-strand breaks and maintain genome stability.
Fig. 1
Don’t Miss: How To Fix Hormonal Imbalance Without Birth Control
Risk Factors For Triple Negative Breast Cancer
A risk factor is a characteristic that increases an individuals chance of getting a certain condition. For example, cigarette smoking is a risk factor for lung cancer. While anyone can receive a diagnosis of triple negative breast cancer, it is more likely to affect the following individuals:
- Those who are younger than age 40
- Those who have the BRCA1 mutation
- Those of African-American or Hispanic descent
Having one or more of these risk factors does not mean developing triple negative breast cancer is for certain, just as not having any of these risk factors doesnt prevent an individual from being diagnosed with this condition.
How Often Does Triple
Targeted therapy allows healthy cells to survive, but chemotherapy can kill normal cells when eliminating the cancer cells. Sixty percent of patients with triple-negative breast cancer will survive more than five years without disease, but four out of ten women will have a rapid recurrence of the disease.
Don’t Miss: How Much Are Male To Female Hormones
Research Performed Three Decades Ago Enhances Targeted Therapy Today
In 1990, Dr. Mary-Claire King, an assistant professor at UC Berkeley, was the first scientist to demonstrate that a gene on chromosome 17q21, named BRCA1 one year later, was responsible for hereditary early-onset breast cancers. In 1994, Drs. Michael Stratton and Richard Wooster in the UK identified BRCA2. Three decades later, mutations in the BRCA1 and BRCA2 genes become a critical indication to enhance the targeted therapy with Olaparib. It tells us that converting research discoveries to patient-impacting benefits takes pretty long. We need to continue to support basic research today so that new therapies can continue to save patients lives in the future.
To recognize Dr. Mary-Claire Kings fundamental contribution to the genetic understanding of cancer, the National Foundation for Cancer Research awarded Dr. Mary-Claire King the Szent-Györgyi Prize for Progress in Cancer Research in 2016 in Washington DC. Learn more about this award and Dr. Mary-Claire Kings research here.
Olaparib offers survival benefits and brings new hopes to patients with early triple-negative breast cancer. As the patients have to be selected by an FDA-approved blood test before the treatment, patients should work with their doctors to determine whether they are eligible for the treatment before receiving the treatment.
Sign up here to receive our monthly e-newsletter featuring healthy living information, stories of inspiration, support resources, cancer prevention tips, and more.
References:
Breast Cancer Hormone Receptor Status
Breast cancer cells taken out during a biopsy or surgery will be tested to see if they have certain proteins that are estrogen or progesterone receptors. When the hormones estrogen and progesterone attach to these receptors, they stimulate the cancer to grow. Cancers are called hormone receptor-positive or hormone receptor-negative based on whether or not they have these receptors . Knowing the hormone receptor status is important in deciding treatment options. Ask your doctor about your hormone receptor status and what it means for you.
Don’t Miss: What Does Testosterone Supplements Do For You
Treatments For Vaginal Dryness
Vaginal dryness and discomfort can be bothersome menopausal symptoms for some women.
Devices that use lasers or other forms of energy to ‘rejuvenate’ vaginal tissue are now being studied as well, although it’s not yet clear how helpful they might be. It’s important to discuss the possible risks and benefits of these treatments with your doctor before deciding if one is right for you.