Breast Cancer And Early Menarche Statistics
One study found that those who reach menarche before the age of 12 have a 23% higher risk of developing breast cancer than those who reach it at the age of 15 or older.
Many breast cancers are hormone receptor-positive, meaning the cancer cells are sensitive to hormones such as estrogen and progesterone. One theory suggests that more prolonged exposure to cyclic hormonal stimulation of the breast tissue accounts for the correlation between early menarche and breast cancer.
One group of researchers found that women with short, numerous menstrual cycles also have a higher risk of breast cancer due to increased cell division during the luteal phase . Data also shows that excessive exposure to exogenous estrogen and progesterone increases the risk more than estrogen alone.
How Do The Hormones Used In Mht Differ From The Hormones Produced By A Womans Body
The hormones used in MHT come from a variety of plants and animals, or they can be made in a laboratory. The chemical structure of these hormones is similar, although usually not identical, to those of hormones produced by womens bodies.
Non-FDA-approved hormone products, sometimes referred to as bio-identical hormones, are widely promoted and sold without a prescription on the Internet. Claims that these products are safer or more natural than FDA-approved hormonal products are not supported by credible scientific evidence. The FDA provides more information about these products on its Menopause page.
Can A Person With A Family History Of Breast Cancer Take Hrt
A 2019 article in the journal Archives of Breast Cancer states that there are no guidelines on the safety of HRT use in those with a family history of breast cancer.
A systematic review from 2021 notes that HRT does not have a relevant effect on the risk of cancer in those who carry the BRCA gene.
Another study from 2018 found that the use of estrogen after surgery to remove the ovaries does not increase the chance of breast cancer in those with the BRCA1 gene. However, they also note that further research is needed on the effect of progesterone-containing HRT.
Breast Cancer Now suggests that a person should speak with a doctor before using HRT if they have inherited a breast cancer gene, such as BRCA1 or BRCA2.
Also Check: Chinese Herbs For Hormonal Acne
What Are The Side Effects Of Hormone Therapy
The side effects of hormone therapy depend largely on the specific drug or the type of treatment . The benefits and harms of taking hormone therapy should be carefully weighed for each person. A common switching strategy used for adjuvant therapy, in which patients take tamoxifen for 2 or 3 years, followed by an aromatase inhibitor for 2 or 3 years, may yield the best balance of benefits and harms of these two types of hormone therapy .
Hot flashes, night sweats, and vaginal dryness are common side effects of all hormone therapies. Hormone therapy also may disrupt the menstrual cycle in premenopausal women.
Less common but serious side effects of hormone therapy drugs are listed below.
Tamoxifen
- breathing problems, including painful breathing, shortness of breath, and cough
- loss of appetite
Combined Hrt And Breast Cancer
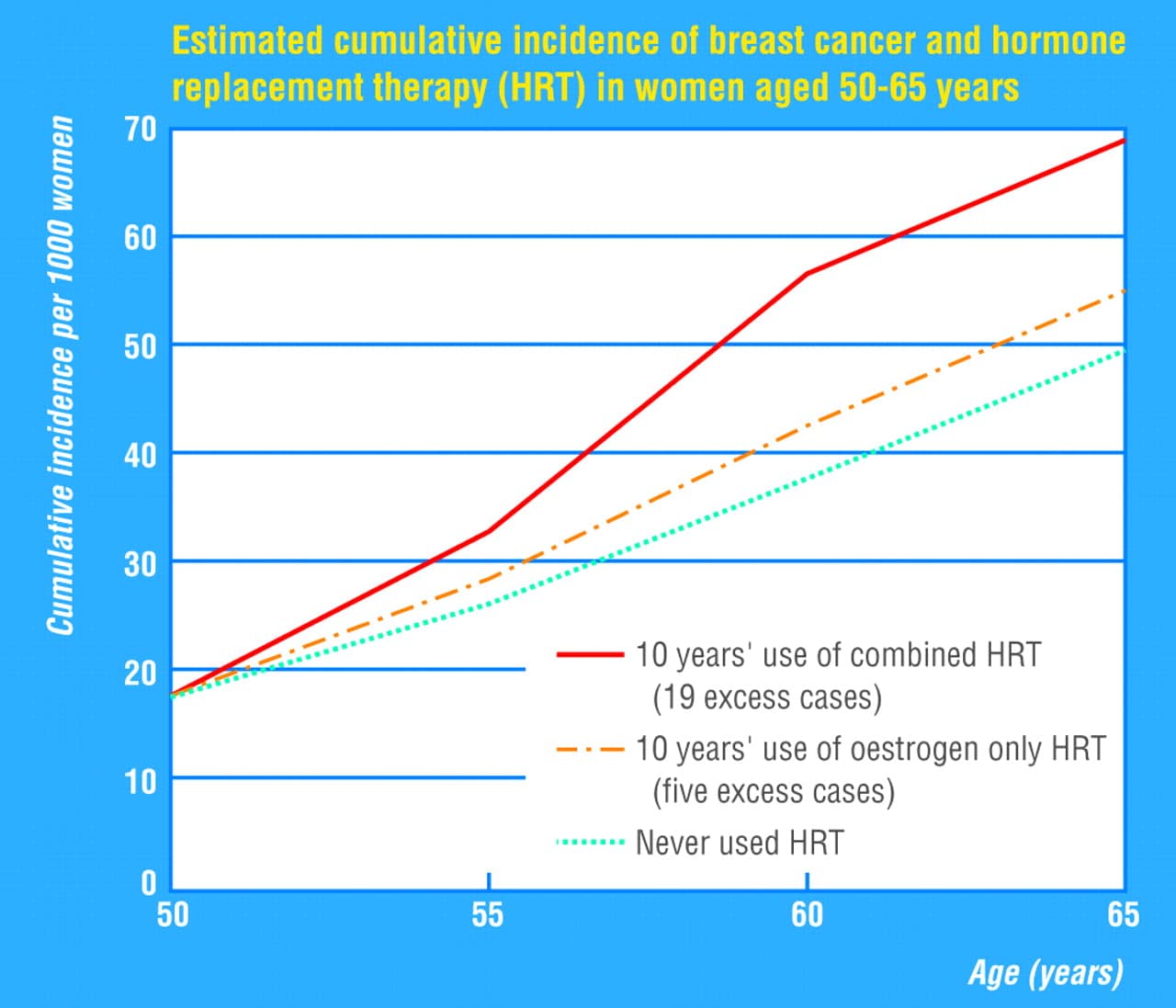
Combined estrogen and progesterone may have the highest risk factor of any type of HRT. According to BreastCancer.org, the risk of developing breast cancer increases by 75% for those taking combined HRT.
The organization also noted that combined HRT increases the chance that a healthcare professional may diagnose a persons breast cancer at a more advanced stage, which increases the likelihood of mortality.
According to the , the risk of breast cancer increases the longer a person takes HRT. However, it also decreases significantly after a person discontinues HRT.
The American Cancer Society states that the risk of breast cancer returns to average 3 years after a person discontinues combined HRT.
However, the researchers for the 2020 study found that risk reduced after 5 years for medroxyprogesterone, and 10 years for levonorgestrel, which are types of progesterone.
Combined HRT is also linked to breast density, which can make it harder to locate cancer on a mammogram. Breast density is a term to describe the amount of dense tissue compared to fatty tissue in a persons breast. Dense tissue is more fibrous than fatty tissue.
HRT containing estrogen alone can also increase the risk of a person developing breast cancer. However, it may only increase the risk after 10 years of continued use.
A person who has had or has breast cancer should not take HRT. Instead, they should speak with a doctor about alternative options.
Don’t Miss: What Is The Most Effective Dose Of Melatonin
Alternatives To Hrt For Protecting Your Bones From Osteoporosis
HRT is no longer recommended for treatment of osteoporosis due to its risks and available alternative options. Bisphosphonate medications are generally recommended to treat osteoporosis instead. Other medications that may be considered are teriparatide, denosumab, or selective estrogen receptor modulators . SERMs are a newer class of drugs, similar to estrogen, that protect against osteoporosis by increasing bone density, while also protecting against the development of breast cancer.
Evista is a widely used SERM that has been shown to increase bone growth and density and reduce the risk of breast cancer. Unfortunately, it does not relieve symptoms of menopause such as hot flashes and may actually worsen them. It is primarily used in women who are at high risk for developing breast cancer or for those who cannot tolerate other medications used to treat osteoporosis.
Additional steps you can take to prevent and/or treat osteoporosis include:
- Performing weight-bearing exercises
Can A Person Lower Their Breast Cancer Risk
If a person decides to take HRT, they can ask for a lower-dose formula. They can also discuss with a doctor how to take it for the shortest possible time.
BreastCancer.org notes that a person can take certain steps to reduce their risk of developing breast cancer whether they use HRT or not.
They recommend that a person:
- exercise regularly
- quit smoking, if applicable
- limit their intake of alcohol
It is also important to achieve and maintain a healthy weight. This is because having more fat tissue can raise a persons estrogen levels, and as a result,
Read Also: Is It Ok To Give Child Melatonin
You May Be Interested To Read
A large-scale study of HRT and the risk of breast cancer: Million Women Study Collaborators. Breast cancer and hormone-replacement therapy in the Million Women Study. The Lancet 2003 362:9382
Menopause: diagnosis and management – National Institute for Health and Care Excellence guidance on diagnosing and managing menopause.
HRT and breast cancer risk: a blog post from the ICR discussing what research about HRT and breast cancer means for women.
Further information on the Breast Cancer Now Generations Study.
Funding: This work is partially funded by the NIHR School for Primary Care Research and by Cancer Research UK through its Oxford Centre.
Conflicts of Interest: The study authors declare no conflicts of interest.
Disclaimer: NIHR Alerts are not a substitute for professional medical advice. They provide information about research which is funded or supported by the NIHR. Please note that views expressed in NIHR Alerts are those of the author and reviewer and not necessarily those of the NHS, the NIHR or the Department of Health and Social Care.
Effect On Risk By Age Of Initiation Of Hrt
The risk of breast cancer depends on many factors, including age at menopause. Women who do not use HRT and who experience menopause between ages 40 and 50 years have a lower risk of breast cancer than women who experience menopause at a later age. However, in women who start HRT in their 40s, the number of HRT-related breast cancers diagnosed by age 69 years is similar to that in women who use HRT for a similar duration starting in their 50s. This is because women who have a menopause in their 40s have longer time as a current HRT-user plus ex-user before they are 69 years old.
It is not known if the increased risk of breast cancer with HRT use is similar for women who take HRT following a premature menopause , or how their risk may be affected by any underlying conditions.
Read Also: What Are Bioidentical Hormones Made From
Cancer Treatment And Bone Thinning In Women
Any cancer treatment in women that lowers oestrogen levels can increase the risk of osteoporosis. These treatments include:
- chemotherapy which causes an early menopause
- radiotherapy to the ovaries which stops them working
- surgery to remove the ovaries before your menopause
- hormone therapy drugs, such as aromatase inhibitors
Osteoporosis Risk And Hormone Therapy
Osteoporosis is thinning of the bones so that they become more brittle. This increases the risk of breaking .
Our bones start to thin after the age of 35 or so, as part of the natural ageing process. But this is not usually noticeable. After the menopause , the levels of the sex hormone oestrogen decrease. This causes bones to lose strength.
Men lose bone strength too, as they age. Because men dont have a menopause, this is usually seen a bit later in life than women.
Hormone therapy and cancer
Some cancers use hormones to grow or develop. Doctors call these cancers hormone sensitive. Hormone therapy works by blocking or lowering the amount of these hormones. For people with breast or prostate cancer, hormone therapy is often an important part of treatment. Ovarian and womb cancer might also be hormone sensitive.
Hormone therapy can increase the risk of bone thinning.
Also Check: How To Get Rid Of Hormonal Breakouts
Incidence Of Breast Cancer
During a median follow-up of 5.35 years , 26,797 women were newly diagnosed with breast cancer. Among them, 92.9% had invasive breast cancer and 7.1% had ductal carcinoma in situ . The HR of the risk of breast cancer in HRT users was 1.25 compared with HRT nonusers. The results of a multivariable analysis of the incidence of breast cancer according to HRT duration are shown in . The incidence of breast cancer significantly increased with increasing HRT duration. The adjusted HRs for breast cancer incidence in women who had used HRT for < 2 years, 2 to < 5 years, and 5 years were 1.08 , 1.33 , and 1.72 , respectively. This proportional increase in the incidence of breast cancer according to HRT duration was evident in women with invasive breast cancer and those with DCIS . The cumulative incidence of breast cancer was linearly related to the duration of HRT .
Adjusted HRs and 95% CIs of the risk of breast cancer according to HRT duration and invasive/in situ breast cancer.
| . |
|---|
Hormone Replacement In Premenopausal Women Treated With Bilateral Oophorectomy For Ovarian Cancer A Nationwide Population
- AffiliationsDepartment of Obstetrics and Gynecology, Danderyd Hospital, Stockholm, SwedenDepartment of Womens and Childrens Health, Division of Neonatology, Obstetrics and Gynecology, Karolinska Institute, Stockholm, Sweden
- Department of Obstetrics and Gynecology, Sahlgrenska University Hospital, Gothenburg, SwedenInstitute of Clinical Sciences, Sahlgrenska Academy at University of Gothenburg, Gothenburg, Sweden
- Department of Reproductive Medicine, Division of Gynecology and Reproduction, Karolinska University Hospital, SwedenDepartment of Oncology-Pathology, Karolinska Institute, Stockholm, Sweden
- Department of Oncology, Institute of Clinical Sciences, Sahlgrenska Academy, University of Gothenburg, SwedenRegional Cancer Centre Western Sweden, Sahlgrenska University Hospital, Gothenburg, Sweden
- Angelique Flöter RådestadAffiliationsDepartment of Womens and Childrens Health, Division of Neonatology, Obstetrics and Gynecology, Karolinska Institute, Stockholm, SwedenDepartment of Hereditary Cancer, Karolinska University Hospital, Stockholm, Sweden
- HRT prescription pick-up is low in women with premature menopause and ovarian cancer.
- < 50% of premenopausal women with ovarian cancer were dispensed HRT after surgical menopause.
- Young age and borderline ovarian tumors were factors that led to a significant dispensing of HRT.
Recommended Reading: Bioidentical Hormone Doctors In Massachusetts
It May Improve Memory Concentration And Cognition
Although there is no hard data to back up the claim, there is some evidence that hormone replacement therapy may be good for you. Indeed, studies have shown that it can lower your risk of Alzheimers disease and other dementias. As a bonus, youll be more productive and happier overall. This is especially true if you consider the long term effects of post-menopausal stress. The best part is, its not as expensive as you might think. Unlike prescription drugs, estrogen can be taken orally, and you can take it as often as you want. Its also a good idea to have your doctor check your blood pressure and cholesterol levels on a regular basis. If youre looking for an inexpensive way to stay young, active, and in top form, then this could be the ticket for you. Thankfully, a growing number of doctors are willing to take a gamble on the untested doctor. One of the more reputable centers is located at the University of California at San Diego. The other is at the University of Southern California in Orange County. In short, these centers are the gold standard in the hormonal treatment industry. They have been researching the topic for over a decade. During this time, they have assembled some incredibly useful information. Hopefully, this will help physicians to more effective prescribing decisions.
Estimates Of Number Of Extra Cases Of Breast Cancer For 5 Years Hrt Use Starting Around The Time Of Menopause
In the UK about 1 in 16 never-users of HRT will be diagnosed with breast cancer between the ages of 50 years and 69 years.
Among women of average weight who start using systemic HRT from menopause in their 40s or 50s, and continue for 5 years, the extra number of cases of breast cancer by age 69 years is estimated from the study to be:
- around 1 extra case per 200 women who use estrogen-only HRT
- around 1 extra case per 70 women who use estrogen combined with progestogen for part of each month
- around 1 extra case per 50 women who use estrogen combined with daily progestogen HRT
The number of extra cases up to age 69 years is approximately double these values for women who use systemic HRT for 10 years compared with those who use HRT for 5 years.
A summary of the numbers of HRT-related breast cancers estimated from the new study, together with other risks and benefits of HRT use, is provided in table 1.
Also Check: Natural Female Hormone Balance Supplements
Lowering Risk Through Early Detection
Breast cancer is the second most common cancer in the United States. Early detection through breast cancer screening increases the chance of survival. The following are breast cancer screening tests:
- Breast exam: Your healthcare provider performs a breast exam to detect any lumps in the breast.
- Mammogram: This is a radiology test of the breast. It’s the most commonly used tool for screening or diagnosis.
- Breast ultrasound: An ultrasound uses sound waves to examine breast tissue. It is often used after a suspicious finding on the mammogram. However, some providers recommend it as a screening tool for women with dense breasts.
Types Of Studies Of Hormone Therapy And Cancer Risk
Different types of studies can be used to look at cancer risk from menopausal hormone therapy .
Randomized controlled trials: In this kind of study, a group of patients get the drug being studied , and another group gets a placebo . Results from this kind of study are powerful because which group a patient is in is based on chance. This helps assure that the groups are similar in all ways, such as risk for cancer, except for the drug thats being studied. This is the best way to see the effects of a drug. These types of studies can also be double-blinded, which means neither the people in the study nor their doctors know which group they are in. This lowers the chance that thoughts or opinions about treatment could affect the study results. Unfortunately, these kinds of studies are costly, which limits the number of people in the study, how long the study can continue, and the number of studies done.
A major drawback of observational studies is that the people getting the treatment being studied may have different cancer risk factors than the people who arent. Plus, the treatment can differ between the people being studied. This makes it less clear that the differences seen are only due to the drug being studied and not other factors.
When observational studies and randomized controlled trials have different results, most experts give more weight to the results of the randomized controlled trial.
Read Also: How To Know When Testosterone Is Low
Types Of Hormone Therapy For Ovarian Cancer
There are different types of ovarian cancer hormone therapy drugs, including:
Luteinizing hormone-releasing hormone agonists. These drugs curb estrogen production in your ovariesâ cells. You might take them if you arenât in menopause.
You get these drugs as shots at your treatment center or doctorâs office. Your doctor may choose to give it to you every 1 to 3 months, depending on the stage and type of cancer you have. LHRH agonist drugs used for ovarian cancer include:
Tamoxifen. You may know of tamoxifen as a breast cancer treatment. It can also be used to treat ovarian stromal tumors, and itâs less likely to be used to treat ovarian epithelial cancer. Tamoxifen works to keep estrogen in your body from helping your cancer grow and spread.
If tamoxifen is part of your treatment plan, youâll get regular tests to check on whether it is working properly and manage any side effects you may have. You shouldnât take tamoxifen if you also take a blood thinner medication such as warfarin.
Research shows that tamoxifen can also raise your risk for other types of cancers like those of the liver, uterus, or endometrium. It can also make blood clots more likely, which can cause serious conditions like deep vein thrombosis . If youâre taking tamoxifen and notice any swelling or pain in your legs, arms, chest, or shortness of breath, tell you doctor right away. If you have a DVT, youâll need immediate treatment.
Aromatase inhibitors include:
Treatment for ovarian cancer will depend on: