How Breast Cancer Is Treated
In cancer care, doctors specializing in different areas of cancer treatmentsuch as surgery, radiation oncology, and medical oncologywork together with radiologists and pathologists to create a patients overall treatment plan that combines different types of treatments. This is called a multidisciplinary team. Cancer care teams include a variety of other health care professionals, such as physician assistants, nurse practitioners, oncology nurses, social workers, pharmacists, counselors, nutritionists, and others. For people older than 65, a geriatric oncologist or geriatrician may also be involved in their care. Ask the members of your treatment team who is the primary contact for questions about scheduling and treatment, who is in charge during different parts of treatment, how they communicate across teams, and whether there is 1 contact who can help with communication across specialties, such as a nurse navigator. This can change over time as your health care needs change.
A treatment plan is a summary of your cancer and the planned cancer treatment. It is meant to give basic information about your medical history to any doctors who will care for you during your lifetime. Before treatment begins, ask your doctor for a copy of your treatment plan. You can also provide your doctor with a copy of the ASCO Treatment Plan form to fill out.
Learn more about making treatment decisions.
Will I Need Chemotherapy After A Total Mastectomy
A total mastectomy is the surgical removal of the entire breast to treat breast cancer. A physician may recommend this treatment on its own or in combination with another therapy, such as chemotherapy. When chemotherapy is provided after surgery, it is called adjuvant chemotherapy. Whether or not chemotherapy is recommended following a total mastectomy will depend on many different factors, including the patients overall health, age and medical history as well as the type, stage and nature of the breast cancer.
Preventing Breast Cancer In The Opposite Breast
About 1 in 20 women diagnosed with breast cancer will develop breast cancer in the opposite breast within the 10 years after first breast cancer diagnosis. A 2017 study in the prestigious medical journal JAMA found that taking tamoxifen can reduce the percentage of those women from developing cancer in the opposite breast within 10 years, from about 5% to 2%. Unfortunately, the study authors did not report on breast cancer deaths or deaths for any other reason. Therefore, we do not know whether tamoxifens reduction of cancer in the opposite breast had any impact on the womens longevity.
Don’t Miss: What Are Hormone Levels In Menopause
When Is Chemotherapy Used
Not all women with breast cancer will need chemo, but there are several situations in which chemo may be recommended:
- After surgery : Adjuvant chemo might be given to try to kill any cancer cells that might have been left behind or have spread but canât be seen, even on imaging tests. If these cells were allowed to grow, they could form new tumors in other places in the body. Adjuvant chemo can lower the risk of breast cancer coming back.
- Before surgery : Neoadjuvant chemo might be given to try to shrink the tumor so it can be removed with less extensive surgery. Because of this, neoadjuvant chemo is often used to treat cancers that are too big to be removed by surgery when first diagnosed . Also, by giving chemo before the tumor is removed, doctors can see how the cancer responds to it. If the first set of chemo drugs doesnt shrink the tumor, your doctor will know that other drugs are needed. It should also kill any cancer cells that have spread but canât be seen. Just like adjuvant chemo, neoadjuvant chemo can lower the risk of breast cancer coming back.
For certain types of breast cancer, if there are tumor cells still found at the time of surgery , you may be offered more chemotherapy after surgery to reduce the chances of the cancer coming back .
Inflammatory Breast Cancer Treatment
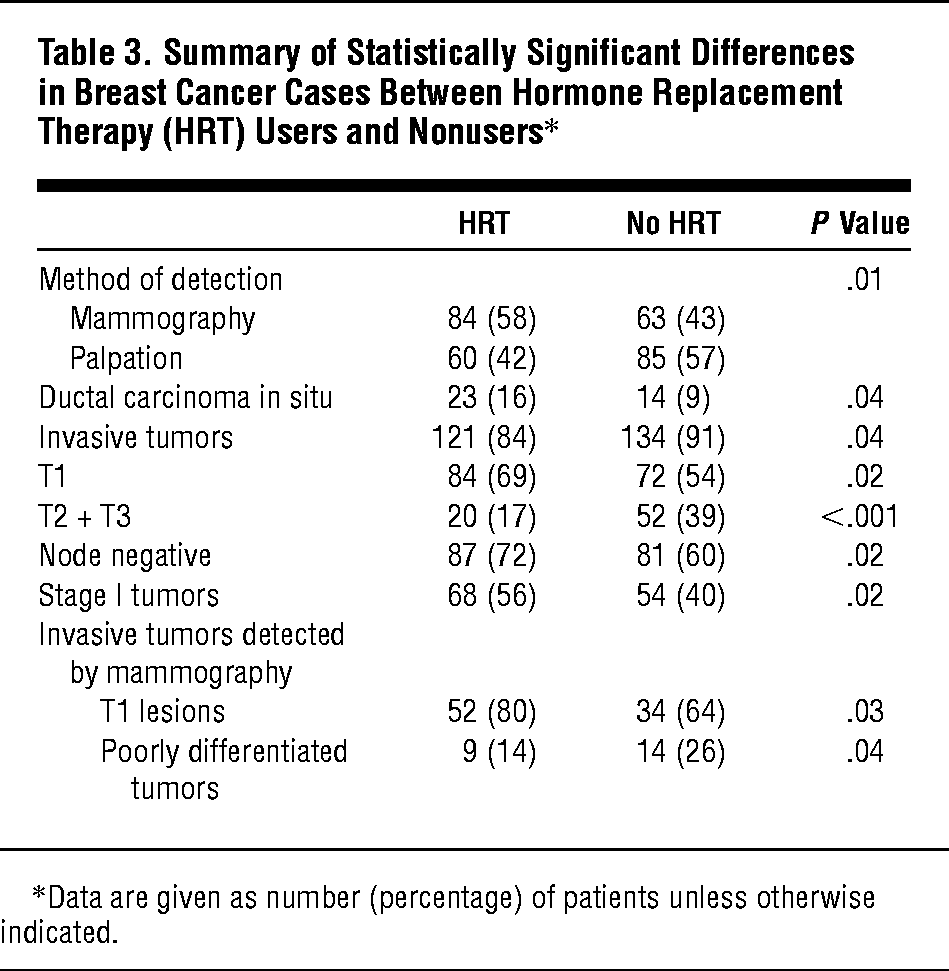
Inflammatory breast cancer is an uncommon and aggressive type of breast cancer caused by cancer cells blocking lymph vessels in the skin.
All IBC cases are classified as at least stage 3 breast cancer. If the cancer is metastatic , its considered stage 4.
Treatments for IBC depend on what stage the cancer is in.
Also Check: How To Treat Hormonal Acne At Home
What Is Hormone Therapy
Hormone therapy slows or stops the growth of hormone-sensitive tumors by blocking the bodys ability to produce hormones or by interfering with effects of hormones on breast cancer cells. Tumors that are hormone insensitive do not have hormone receptors and do not respond to hormone therapy.
Hormone therapy for breast cancer should not be confused with menopausal hormone therapy treatment with estrogen alone or in combination with progesterone to help relieve symptoms of menopause. These two types of therapy produce opposite effects: hormone therapy for breast cancer blocks the growth of HR-positive breast cancer, whereas MHT can stimulate the growth of HR-positive breast cancer. For this reason, when a woman taking MHT is diagnosed with HR-positive breast cancer she is usually asked to stop that therapy.
Ovarian Ablation Or Suppression
In women who have not yet experienced the menopause, oestrogen is produced by the ovaries.
Ovarian ablation or suppression stops the ovaries working and producing oestrogen.
Ablation can be done using surgery or radiotherapy. It permanently stops the ovaries from working and means you’ll experience the menopause early.
Ovarian suppression involves using a medicine called goserelin, which is a luteinising hormone-releasing hormone agonist .
Your periods will stop while you’re taking it, although they should start again once your treatment is complete.
If you’re approaching the menopause , your periods may not start again after you stop taking goserelin.
Goserelin comes as an injection you have once a month.
Don’t Miss: How To Get Prescribed Testosterone
Benefits Of Hormone Therapies In Early And Locally Advanced Breast Cancer Treatment
Treatment with the hormone therapies tamoxifen and/or an aromatase inhibitor lowers the risk of :
- Breast cancer recurrence
- Breast cancer in the opposite breast
- Death from breast cancer
Premenopausal women who get ovarian suppression plus tamoxifen or an aromatase inhibitor may lower these risks more than premenopausal women who get tamoxifen or an aromatase inhibitor alone .
Learn more about tamoxifen.
|
Aromatase inhibitor plus androgen deprivation therapy |
How Radiation Is Used With Other Cancer Treatments
For some people, radiation may be the only treatment you need. But, most often, you will have radiation therapy with other cancer treatments, such as surgery, chemotherapy, and immunotherapy. Radiation therapy may be given before, during, or after these other treatments to improve the chances that treatment will work. The timing of when radiation therapy is given depends on the type of cancer being treated and whether the goal of radiation therapy is to treat the cancer or ease symptoms.
When radiation is combined with surgery, it can be given:
- Before surgery, to shrink the size of the cancer so it can be removed by surgery and be less likely to return.
- During surgery, so that it goes straight to the cancer without passing through the skin. Radiation therapy used this way is called intraoperative radiation. With this technique, doctors can more easily protect nearby normal tissues from radiation.
- After surgery to kill any cancer cells that remain.
Don’t Miss: How To Free Up Testosterone
Risk Of Late Recurrence Is Underestimated
A survey led by the Canadian Breast Cancer Network found that women often underestimate their risk of late recurrence. In the survey, only 10% were aware of the risk of recurrence after five years of tamoxifen therapy, and 40% felt that they were cured after hitting the five-year mark.
Many breast cancer survivors underestimate their risk of late recurrence.
Read Also: What Do Breast Cancer Patients Need
When Is Hormone Therapy Used For Breast Cancer
Hormone therapy is often used after surgery to help reduce the risk of the cancer coming back. Sometimes it is started before surgery .
It is usually taken for at least 5 years. Treatment longer than 5 years might be offered to women whose cancers have a higher chance of coming back. A test called the Breast Cancer Index might be used to help decide if a woman will benefit from more than 5 years of hormone therapy.
Hormone therapy can also be used to treat cancer that has come back after treatment or that has spread to other parts of the body.
Read Also: What’s The Highest Dose Of Melatonin You Can Take
Possible Side Effects Of Ais
The most common side effects of AIs are:
- Bone and joint pain
AIs tend to have side effects different from tamoxifen. They don’t cause uterine cancers and very rarely cause blood clots. They can, however, cause muscle pain and joint stiffness and/or pain. The joint pain may be similar to a feeling of having arthritis in many different joints at one time. Options for treating this side effect include, stopping the AI and then switching to a different AI, taking a medicine called duloxetine , or routine exercise with nonsteroidal anti-inflammatory drugs . But the muscle and joint pain has led some women to stop treatment. If this happens, most doctors recommend using tamoxifen to complete 5 to 10 years of hormone treatment.
Because AIs drastically lower the estrogen level in women after menopause, they can also cause bone thinning, sometimes leading to osteoporosis and even fractures. If you are taking an AI, your bone density may be tested regularly and you may also be given bisphosphonates or denosumab , to strengthen your bones.
Risk Factors For Overall Recurrence
There are several risk factors that raise the risk of recurrence overall . These include:
- Tumor size: Larger tumors are more likely to recur than smaller ones both early and late.
- Positive lymph nodes: Tumors that have spread to lymph nodes are more likely to recur at any time than those that have not.
- Age at diagnosis: Breast cancer recurrence is more common in younger people.
- Treatments received and response to treatments: Both chemotherapy and hormonal therapy reduce the risk of recurrence in the first five years.
- Tumor grade: More aggressive tumors are more likely to recur than less aggressive tumors , especially in the first five years
There are also factors that do not appear to affect the risk of recurrence. Recurrence rates are the same for women who have a mastectomy or lumpectomy with radiation and are also the same for women who have a single vs. double mastectomy.
Recommended Reading: How To Increase Estrogen Naturally Dr Axe
Breast Cancer May Return Even 20 Years Later Researchers Find
This means women with the most common type of breast cancer, called estrogen-positive or hormone-positive breast cancer, need to think carefully about whether they want to stop taking the pills, even if they cause side-effects, doctors said.
These breast cancers have a lingering smoldering quality and carry substantial risk of late recurrence after five years of therapy, said Dr. Harold Burstein of the Dana Farber Cancer Institute, who was not involved in the study.
Many patients think. OK, I made it to five years. I know Im safe, said Dr. Jennifer Litton, an oncologist at the MD Anderson Cancer Center. But for estrogen-receptor positive breast cancer, its a continued lifelong risk.
Related: Breast Cancer Drug Can Also Prevent Cancer
Breast cancer is the second-biggest cancer killer of American women, after lung cancer. The American Cancer Society says every year, itâs diagnosed in 200,000 women and a few men, and kills around 40,000.
Most breast cancers are fueled by estrogen, and drugs called hormone blockers are known to cut the risk of recurrence in such cases.
Tamoxifen long was the top choice, but newer drugs called aromatase inhibitors sold as Arimidex, Femara, Aromasin and in generic form do the job with less risk of causing uterine cancer and other problems. The longer women take them, the lower their risk of having the cancer come back.
However, they do cause side-effects.
Related: Gel Works As Well As Pill to Prevent Breast Cancer
Hormone Therapy For Breast Cancer
Some types of breast cancer are affected by hormones, like estrogen and progesterone. The breast cancer cells have receptors that attach to estrogen and progesterone, which helps them grow. Treatments that stop these hormones from attaching to these receptors are called hormone or endocrine therapy.
Hormone therapy can reach cancer cells almost anywhere in the body and not just in the breast. It’s recommended for women with tumors that are hormone receptor-positive. It does not help women whose tumors don’t have hormone receptors .
Read Also: What’s The Best Hormone Replacement Therapy
How Does Hormone Therapy Work
About 2 out of 3 breast cancers are hormone receptor-positive. Their cells have receptors for estrogen and/or progesterone which help the cancer cells grow and spread.
There are several types of hormone therapy for breast cancer. Most types of hormone therapy either lower estrogen levels in the body or stop estrogen from helping breast cancer cells grow.
The Myth And Stigma Of The 5
Many people still believe that breast cancer, even hormone-positive disease, is essentially cured after five years this can lead to misunderstandings in families. Loved ones who donât understand late recurrence may downplay your feelings, or criticize you when you think âbrain tumorâ each time you get a headache.
Until information on late recurrence becomes more widely known, and even though itâs frustrating, you may need to educate loved ones about the risk, and why you should be concerned when you develop new or unexplained symptoms.
Read Also: Can You Work During Breast Cancer Treatment
Recommended Reading: Hormone Tablets For Breast Cancer Side Effects
Prognosis Of Late Vs Early Cancer Recurrence
Late recurrence is associated with a better prognosis than early recurrence in estrogen receptor-positive breast cancer. A 2018 study in Clinical Breast Cancer found that survival after recurrence was significantly longer in people with a late versus early recurrence . In this study, the lungs were the most common site of late distant recurrence.
Enhancing Healthcare Team Outcomes
Breast cancer still remains a common malignancy in females, and although there are reports that the incidence is declining in certain countries, prompt diagnosis and treatment are necessary to prevent morbidity and mortality. The management of breast cancer is by an interprofessional team that includes an oncologist, surgeon, radiation oncologist, a pathologist, and an oncologic nurse. With a higher emphasis on breast-conserving surgery followed by radiation, many studies report favorable results. Further, many techniques have been developed to deliver radiation to the breast and studies have shown that the risk of recurrence outside the excised lesion is similar whether the whole or partial breast is treated. The treatment of breast cancer continues to evolve, and there are now studies trying to determine the feasibility of delivering radiation intraoperatively. Because breast cancer is a heterogeneous disorder, the key is proper patient selection to achieve the highest cure rates with the least morbidity.
Don’t Miss: Is Birth Control Hormone Replacement Therapy
Types Of Hormonal Therapies For Early Stage Breast Cancer
Hormonal therapy is the opposite of the type of hormones women sometimes take to reduce the symptoms of menopause. It lowers your estrogen levels instead of increasing them.
Hormonal therapy is recommended for most women with breast cancer, and sometimes it is taken by women who have not been diagnosed with breast cancer but are at high risk for it based on their genes or family history. When hormonal therapy is used before breast cancer develops, it is called primary prevention or chemoprevention. Chemoprevention is completely different from the drugs used in chemotherapy to treat breast cancer. See our article on breast cancer prevention.
What Are Hormone Inhibitors And How Do They Work
Hormone inhibitors also target breast cancer cells with hormone receptors, but unlike hormone blockers, they work by reducing the bodys hormone production. When breast cancer cells are cut off from the food supply the tumor begins to starve and die.Generally, the benefits of using hormone therapy and chemotherapy together have a much greater combined effect than using either alone. If your breast cancer is positive for hormone receptors, your doctor may recommend both therapies.
Read Also: How To Get Rid Of Hormonal Cystic Acne On Chin
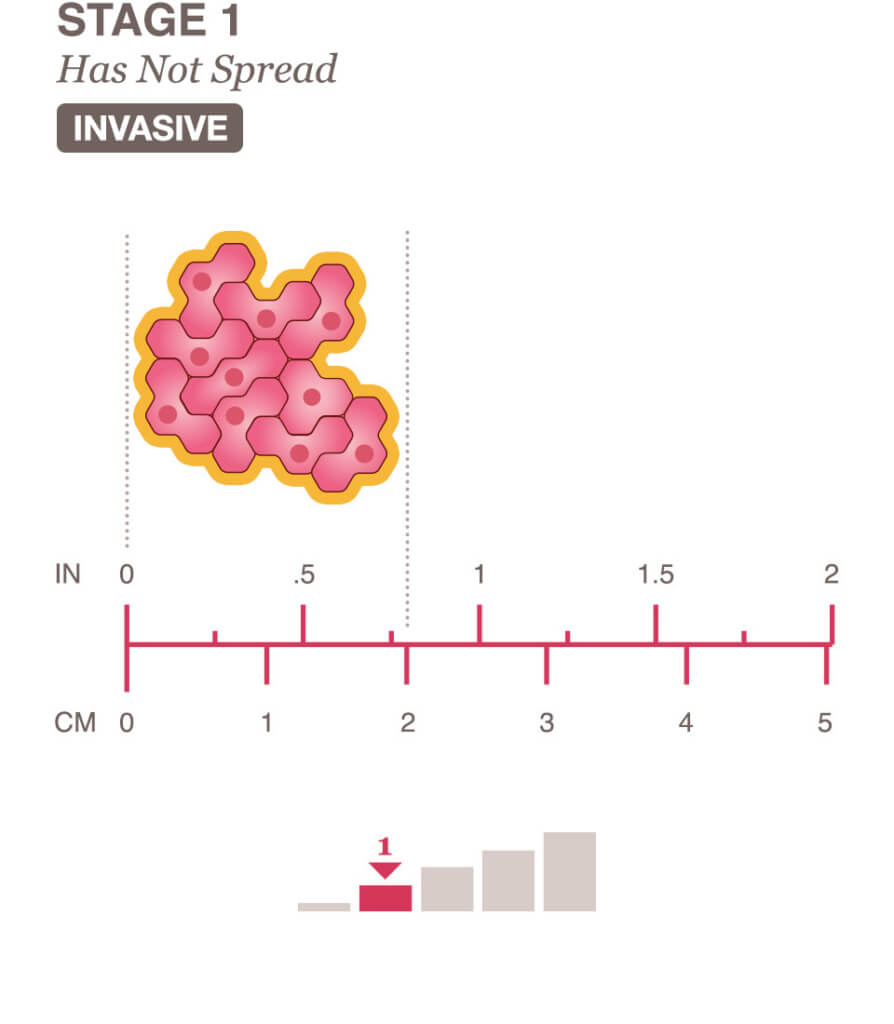
Stage 1 Breast Cancer: Treatment And Prognosis
Breast cancer is classified into different stages ranging from 0 to 4. Staging is based on the tumors size and whether tumor cells have spread to other parts of the body. Determining your cancers stage can help your doctor determine your prognosis and the best treatment options.
The TNM staging system which stands for tumor, node, and metastasis is generally used for breast cancer staging. The system stages tumors based on:
- Tumor How large is the primary tumor?
- Node Are there cancer cells in lymph nodes?
- Metastasis Has the cancer metastasized, or spread, to other parts of the body?
Each letter is assigned a number, often with a letter following it. A lower number corresponds to early stage breast cancer, and a higher number indicates more advanced breast cancer.
Other information is also used to better understand the stage of the cancer. This can include:
- Hormone receptor status Whether the cancer contains estrogen receptors or progesterone receptors, proteins that respond to hormones in the body
- Tumor grade A measure of how abnormal the cancer cells look compared to normal cells
- HER2 status Whether the cancer has high levels of a protein called HER2
- Oncotype DX score Results of a genetic test used to predict if a cancer might progress to a more serious form of cancer
Following breast cancer diagnosis, a doctor will determine the most effective treatment based on the cancers stage.