Is Pcos Linked To Other Health Problems
Yes, studies have found links between PCOS and other health problems, including:
- Diabetes. More than half of women with PCOS will have diabetes or prediabetes before the age of 40.4 Learn more about diabetes on our Diabetes page.
- High blood pressure. Women with PCOS are at greater risk of having high blood pressure compared with women of the same age without PCOS. High blood pressure is a leading cause of heart disease and stroke. Learn more about heart disease and stroke.
- Unhealthy cholesterol. Women with PCOS often have higher levels of LDL cholesterol and low levels of HDL cholesterol. High cholesterol raises your risk of heart disease and stroke.
- Sleep apnea. This is when momentary and repeated stops in breathing interrupt sleep. Many women with PCOS have overweight or obesity, which can cause sleep apnea. Sleep apnea raises your risk of heart disease and diabetes.
- Depression and anxiety.Depression and anxiety are common among women with PCOS.
- Endometrial cancer. Problems with ovulation, obesity, insulin resistance, and diabetes increase the risk of developing cancer of the endometrium .
Researchers do not know if PCOS causes some of these problems, if these problems cause PCOS, or if there are other conditions that cause PCOS and other health problems.
Effect Of Androgen At Physiological Levels On Bone In Women
Estrogen has been shown to increase bone mass in men and women . Similarly, androgen receptors are expressed on the surface of all the three bone cells, osteoblast, osteoclast and osteocyte in both men and women indicating the direct influence of androgen on bone. Shimodaira and coworkers , demonstrated that osteoblasts of the MG-63 and HOS cell lines possess both 5a-reductase and aromatase activities. Dihydrotestosterone is a potent non-aromatizable androgen. 5a-reductase will convert testosterone to DHT. DHT helps in the proliferation and differentiation of osteoblast cells . But whether level of 5a-reductase is elevated in the osteoblast cell of PCOS subjects is not yet studied.
Schematic representation showing the effects of androgen/ on BMD. AC, adenylate cyclase cAMP, cyclic adenosine mono phosphate PKA, Protein kinase A DHEA, dehydroepiandosterone. A full colour version of this figure is available at .
Citation: Journal of Endocrinology 232, 2 10.1530/JOE-16-0405
The LH stimulation of androgen synthesis appears to be augmented by factors such as inhibin and downregulated by factors such as activin, epidermal growth factor , TGF and TGF. Inhibin also inhibits FSH secretion. It was suggested that inhibin B from multiple small viable follicles should also cause increased LH and decreased FSH secretion .
Hyperinsulinemia And Insulin Resistance
Insulin resistance is defined as a pathological condition in which a cell, tissue or organism requires above-normal quantities of insulin to respond normally. It causes increased insulin secretion by pancreatic cells and compensatory hyperinsulinemia, while blood glucose remains normal. When the response of pancreatic cells decreases, the patient develops glucose intolerance or type II diabetes .
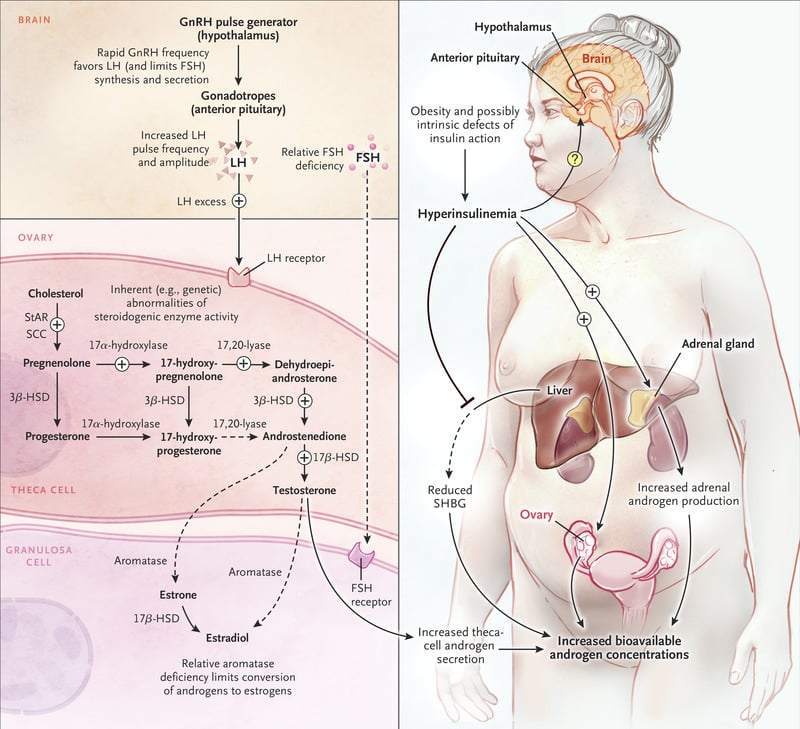
Since many women with PCOS seem to have insulin resistance, compensatory hyperinsulinemia is thought to contribute to hyperandrogenism by direct stimulation of ovarian production of androgens and by inhibition of liver synthesis of SHGB that increases testosterone availability. Insulin also increases ACTH-mediated adrenal androgen production and accentuates LH-stimulated ovarian steroidogenesis .
Hyperinsulinemia stimulates directly cytochrome p450 enzymes in the ovary or indirectly through action of LH or IGF-1, causing hyperandrogenism
In vitro data, obtained with cell culture models, indicate that co-incubation of insulin and FSH with bovine oocytes promotes up-regulation of LH receptors on granulosa cells of antral follicles. It contributes to arrest of follicular growth, inhibits of aromatase activity, and potentially triggers to ovarian hyperandrogenism. Looking at the molecular level, insulin binds to its receptor on granulosa and thecal cells and on oocytes where it may alter expression of certain genes involved in the meiotic process of the oocyte .
You May Like: Can Pregnancy Hormones Cause Depression
What Are The Signs And Symptoms Of Polycystic Ovary Syndrome
Polycystic ovary syndrome commonly causes problems relating to menstrual periods. They can become erratic, infrequent, or even stop altogether and this can cause reduced fertility. Other symptoms can include greasy skin or acne and there is often an increase in hair growth in a male pattern , which some women may find distressing. Symptoms get worse with weight gain.
Genes Associated With Pcos
You may develop PCOS if you inherit the risk for it from your family. Not only is it true for PCOS, there are other metabolic abnormalities that you might have the risk of developing if your family members have it.
However, you should know that there is no single gene that is linked to PCOS. Because of the complex nature of this chronic illness, there are multiple genes that work in a delicate manner, and abnormalities in these mechanisms can lead to the multiple symptoms we see in women with PCOS. Your genes may also malfunction and affect the levels of your hormones and cause insulin resistance.
There are many studies that confirm that insulin resistance occurs in women with PCOS, even if they do not have an increase in their weight. This can mean that weight and its fluctuations may not be the only reason behind the problem of insulin resistance in women with PCOS.
Recommended Reading: How To Tell If Your Hormones Are Balanced
Understanding Polycystic Ovary Syndrome
Imagine having unusual body hair, irregular periods, or constantly having difficulty losing weight or conceiving women who suffer from Polycystic Ovary Syndrome deal with just a few of these symptoms and more. PCOS is an endocrine disorder comprised of a set of symptoms due to heightened androgens, which are male hormones in women. PCOS is the most common endocrine disease, which affects different endocrine glands in the body, and affects approximately two to twenty percent of women between eighteen to forty-four. The condition is also one of the leading causes of reduced fertility in women.
What Else Do I Need To Know
Its important to follow-up regularly with your health care provider and make sure you take all the medications prescribed to regulate your periods and lessen your chance of getting diabetes or other health problems. Because you have a slightly higher chance of developing diabetes, your health care provider may suggest that you have your blood sugar tested once a year, or have a glucose challenge test every few years. Quitting smoking will also improve your overall health. Because you have a higher chance of developing diabetes, your health care provider may suggest having a:
- Blood sugar test once a year
- A1C test once a year
- Glucose tolerance test every few years
Additional Resources
Chat with us! Our PCOS chats are safe places for teens and young women who share a common condition to ask questions, discuss concerns, and offer each other support.
Getting Treatment: The Reproductive Endocrine Practice at Boston Childrens Hospital offers special services in the diagnosis and treatment of Polycystic Ovary Syndrome . Request an appointment online.
PCOS Resource Book: Our PCOS Resource Book is filled with teen-friendly information about PCOS, including information about what causes PCOS and ways to treat it. The book contains a collection of informational guides, practical tips, worksheets, and recipes to help with PCOS management. You can access the booklet online.
Recommended Reading: Hormone Receptor Breast Cancer Prognosis
Pcos And Hormones: Answers To Frequently Asked Questions
Did you know that 1 in 10 women have polycystic ovary syndrome in their childbearing years? Once you develop PCOS, you may experience metabolism problems and hormonal imbalances. When left untreated, this condition may affect your appearance and overall health.
Understanding how PCOS and hormones relate is crucial if youre suffering or have someone suffering from this disorder. Your body is likely to produce abnormally high levels of male hormones. You may also experience fertility problems and delayed menstrual periods.
You wouldnt want to develop long-term health conditions like heart disease and diabetes from an untreated case of PCOS. We prepared this guide to help you understand how this disorder affects hormones. Here are the FAQs and answers you should know about PCOS.
How Is Polycystic Ovarian Syndrome Treated
Your healthcare provider will determine treatment based on your symptoms, medical history and other health conditions, and if you want to get pregnant. Treatments can include medications, lifestyle changes or a combination of both.
If you do not plan to become pregnant, treatments include:
- Hormonal birth control: Options include birth control pills, patches, shots, a vaginal ring or an intrauterine device . Hormonal birth control helps to regulate your menstrual cycle, improve acne and help with excess hair growth.
- Insulin-sensitizing medicine: Metformin is a drug used to treat diabetes. It works by helping your body process insulin. Once insulin is managed, some people with PCOS see improvements in their menstrual cycles.
- Medications to block androgens: Some drugs can block the effect of androgens. This helps control acne or hair growth caused by PCOS. Talk to your healthcare provider about whether they’re right for you.
- Lifestyle changes: Losing weight and eating a healthy diet can have a positive effect on insulin levels.
If you want to become pregnant now or in the future, treatment for PCOS includes:
You May Like: How To Fix Low Testosterone
Causes Of Pcos Continued
As a complex multigenic condition, the exact affected gene has not yet been discovered. However, it is known the phenotype – the genetic code that creates the condition – appears to manifest itself partially due to the high levels of the androgen present in the ovarian follicle theca cells. As the ovaries are the primary organ affected, recent research has indicated PCOS is a multisystem disorder, with the predominate issue being in the hormonal regulation in the hypothalamus, that includes many organs. Polycystic ovaries develop when a woman’s ovaries are stimulated to produce more hormones, specifically testosterone, by either one or a combination of the release of excessive luteinizing hormone through high levels of insulin in the blood or by the anterior pituitary gland.
Lutenizing Hormone And Follicle Stimulating Hormone
LH levels in PCOS are one of the first things that are measured when this condition is suspected. Both, LH and FSH, are involved in the process of ovulation as they encourage it. These hormones are secreted by the pituitary gland which is located in the brain. To understand how the LH levels in PCOS might get affected, it is also important to take a look at what the normal levels might look like. At the beginning of the cycle, LH and FSH hormones might fall in the range of 5-20mlU/ml often present in equal amounts. However, 24 hours before ovulation, there is a surge in the LH levels and the hormone rises to 25-40mlU/ml. Following the release of the egg, the LH levels go back down.
The difference with PCOS is that even though both these hormones might still be in their optimal range, the LH levels in PCOS are often two or three times higher than FSH. For example if the FSH level is around 6mlU/ml the LH levels in PCOS would be 18mlU/ml.
Recommended Reading: Does Low Estrogen Cause Headaches
What Is Polycystic Ovarian Syndrome
Polycystic ovarian syndrome is a hormonal imbalance caused by the ovaries creating excess male hormones. If you have PCOS, your ovaries produce unusually high levels of hormones called androgens. This causes your reproductive hormones to become imbalanced. As a result, people with PCOS often have erratic menstrual cycles, missed periods and unpredictable ovulation. Small cysts may develop on your ovaries due to lack of ovulation . However, despite the name “polycystic,” you do not need to have cysts on your ovaries to have PCOS.
PCOS is one of the most common causes of female infertility. It can also increase your risk for other health conditions. Your healthcare provider can treat PCOS based on your symptoms and if you have plans for having children.
What Are The Causes And Risk Factors Of Pcos
Doctors donât know all of the reasons why some people get PCOS.
You might be more likely to have PCOS if your sister or mother also has it. It could also be related to problems that make your body produce too much insulin, which can affect your ovaries and their ability to ovulate . Long-term low-grade inflammation may also play a role. White blood cells produce substances to fight infection, and that can cause the ovaries to produce androgens. Most people with PCOS have high levels of androgens.
Transgender men are highly prone to getting PCOS. Hormone therapy may or may not be a factor in that. Thatâs because so many other things â including insulin resistance, metabolic syndrome, and high levels of androgens â come into play with PCOS. In fact, some studies have shown that while hormone therapy can cause changes to the ovaries in transgender men, it doesnât necessarily cause PCOS.
Read Also: Home Hormone Test Kit Male
Myths And Truths About Pcos
There are many misconceptions about PCOS that cause confusion, misdiagnosis, and mistreatment in women who are experiencing the multitude of symptoms associated with the disorder.
Despite the name polycystic ovarian syndrome, having cystic ovaries isnt a requirement to be diagnosed with PCOS.
In fact, the NIH has concluded that the name PCOS should be changed, as the name causes confusion and doesnt reflect the complex metabolic, hypothalamic, pituitary, ovarian, and adrenal interactions that characterize the syndrome.
Many people, including healthcare professionals, also dont even realize that being overweight is not a requirement of having PCOS. Its estimated that one-third to one-half of women with PCOS are at normal weight or underweight and that being overweight or obese does not increase the risk of developing the condition.
While weight loss in women who are overweight may be beneficial, this recommendation isnt useful for women with PCOS symptoms who arent overweight. And using birth control pills as a treatment for amenorrhea is often unnecessary and simply masks a deeper diet and lifestyle problem.
Pcos Continues After Menopause
PCOS is considered a lifelong condition and needs to be managed even after fertility ends.
People without PCOS go through similar changes when they reach perimenopause and menopause as people with PCOS. Factors associated with PCOS commonly appear during perimenopause for people who don’t have PCOS. These include:
- Increasing insulin resistance
- Irregular or absent periods
- Symptoms such as facial hair growth
However, people with PCOS tend to experience these changes earlier, often before perimenopause and, therefore, are exposed to these risk factors for a longer amount of time.
You May Like: What Is Testosterone In Men
What Are The Symptoms And Signs Of Pcos
The symptoms and signs of PCOS can differ between women, and vary in severity and change over time. Symptoms and signs can include:
-
Irregular periods
-
Excess hair growth on face and body
-
Loss or thinning of hair on scalp
-
Darkened patches of skin on the neck or under the arms
-
Difficulty managing weight
-
High cholesterol levels and altered blood lipid profiles
These signs and symptoms can lead to other health issues, including:
-
Fertility problems or difficulties getting pregnant
-
Gestational diabetes
-
Sleep apnoea and sleep difficulties
-
Eating disorders and disordered eating
-
Body image issues
-
Depression, anxiety and mood changes
-
Increased risk of type 2 diabetes
-
Increased risk of cardiovascular disease
-
Increased risk of endometrial cancer
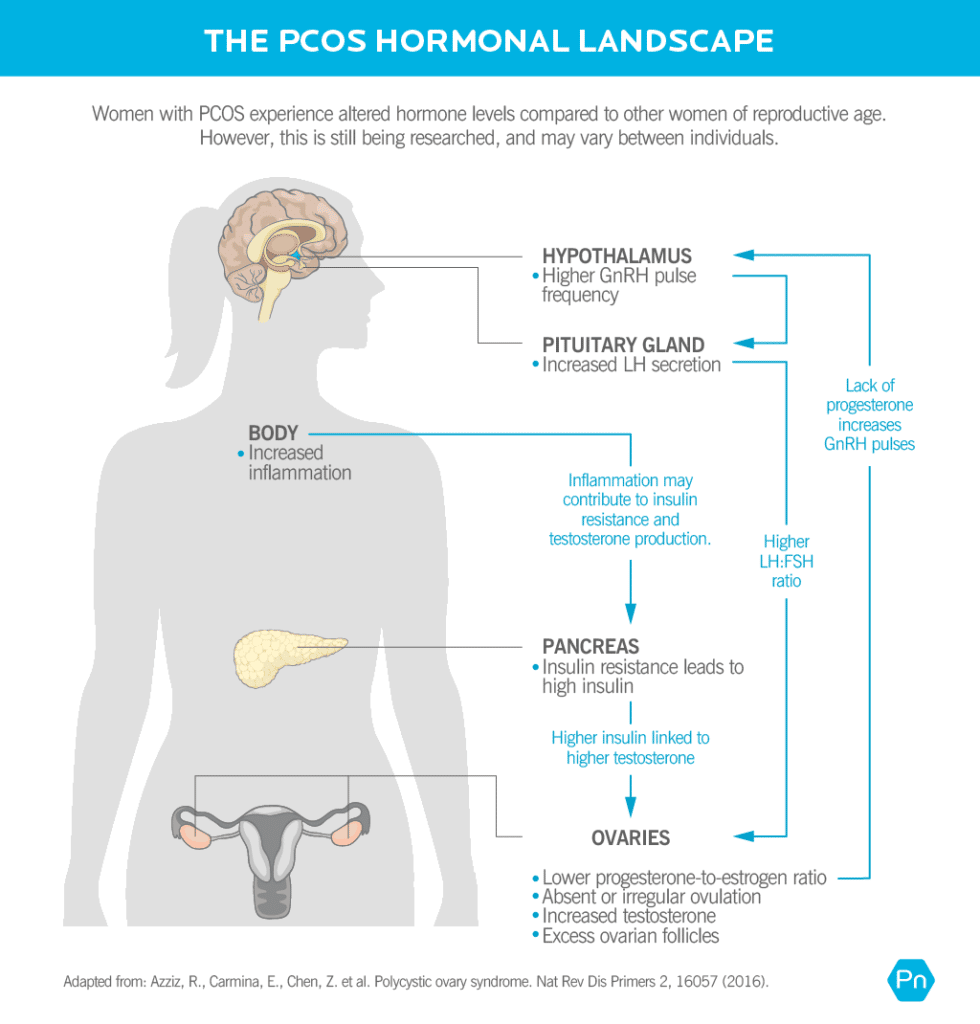
The symptoms of PCOS are caused by the following hormonal imbalances in women with PCOS.
Pcos Causes And Risk Factors
So what causes PCOS? Scientists and physicians use the word syndrome and not disease for PCOS because we do not yet know the exact cause of this condition. We do know that PCOS results from complex interactions between the, androgens, other hormones, and insulin. These complicated interactions of hormones lead to hormone imbalance, growth of cysts on the ovaries, and ineffective insulin . Because the insulin is ineffective, the body produces more of it, and the excess insulin causes a cascade of complications including a high risk of developing and high cholesterol.
Women with PCOS also often make extra androgens, including testosterone. Androgens are typically thought of as male hormones but are present in both men and women.
While the cause of PCOS is unknown, certain factors can put you at higher risk of developing it. Women who are obese or who have a family history of PCOS have a greater likelihood of developing PCOS compared to other women.
You May Like: Hormone Type 6 Meal Plan
Pcos May Increase Your Risk Of Cvd And Diabetes
People with PCOS have an increased risk of cardiovascular disease and type 2 diabetes. It’s unclear whether PCOS directly causes these conditions or if they are due to common risk factors such as obesity.
Most of the research on these increased risks have focused on premenopausal and perimenopausal people. It generally supports the existence of an increased risk for metabolic and cardiovascular disease in people with PCOS, particularly those with extra body fat.
Research on menopausal and postmenopausal people indicate that these risk factors continue past menopause, but the extent to which people with PCOS are at a higher risk than their non-PCOS peers has not been well-established.
This effect is not because the risks go down for people with PCOS, but rather because those without PCOS “catch up” as they age.
There may be some cases in which the risks do decline. One longitudinal study found that people with PCOS whose periods became more regular as they aged had a decrease in their LDL cholesterol and had an improvement in their cardiovascular risk.
The same study found that people with PCOS who remained anovulatory had increases in total cholesterol, LDL cholesterol, and non-high-density lipoprotein cholesterol levels . Their cardiovascular risk remained significantly higher than in the general population.