Key Points: Urogenital Atrophy
-
1. Urogenital atrophy has been newly renamed as GSM, which includes all the symptoms caused by changes in the contraction of the bladder, urethra, vagina, and genitalia due to the decreased estrogen level during menopause and vaginal atrophy.
-
2. The use of topical estrogen is recommended for the treatment of GSM and recurrent UTIs.
-
3. Lubricants, vaginal moisturizers, ospemifene, and vaginal DHEA are non-estrogen therapies available for treating urogenital atrophy, but laser therapy could be considered an additional therapy.
-
4. For menopausal women with symptoms of an overactive bladder, the primary drug therapy is the combination therapy of an antimuscarinic drug and topical estrogen.
-
5. Systemic ET is effective for treating vaginal atrophy but not effective for treating recurrent UTIs, overactive bladder, and urinary incontinence.
Does It Cause Weight Gain
Some people worry that hormone treatment might lead to weight gain, but there is no evidence to support this.
Eating a healthful diet and getting plenty of exercise can help manage the weight gain that commonly affects both females and males in midlife.
There are various ways of delivering hormone therapy, and the different types provide different combinations and amounts of hormones.Common types include:
Estrogen-only HRT: A doctor may recommend this if a person has had their uterus and ovaries removed, in which case progesterone is not necessary.
Cyclical, or sequential, HRT: This may be a good option if symptoms occur before menopause the dosage can align with the menstrual cycle.
Continuous HRT: After menopause, a doctor may prescribe a continuous combination of estrogen and progesterone.
Local estrogen: Vaginal tablets, creams, or rings can help with urogenital symptoms, including vaginal dryness and irritation.
The doctor will prescribe the lowest possible dosage that addresses the persons symptoms, and arriving at this dosage may take some trial and error.
Ways of delivering HRT include:
- tablets
- vaginal rings
- skin patches
When a person no longer needs the treatment, the doctor will describe how to stop it gradually.
Various lifestyle adjustments can help manage the symptoms of menopause.
They include:
Also, it is a good idea to ask the doctor about nonhormonal treatment options.
Always speak to a doctor before using any supplements.
Offers Protection Against Cardiovascular Disease
Numerous studies have confirmed that when HRT is started early, within 10 years of menopause, it can help protect your heart and vascular system from disease.
Before starting HRT, its important to undergo a physical exam to be sure you dont already have signs of cardiovascular disease. Your doctor will likely want you to have a check-up every year while youre on HRT to be sure youre maintaining good heart health.
Also Check: Does Blue Cross Blue Shield Federal Cover Testosterone Therapy
Benefits Of Postmenopausal Hormone Therapy
Among the various hormonal imbalance symptoms that can be alleviated with hormone replacement after menopause are:
- Local irritation
- Among others
Side effects should be reported to an overseeing doctor as soon as possible. Dosages may be reduced, or a different treatment type may be pursued depending upon their severity, among other options.
Hrt Does Not Cause Weight Gain
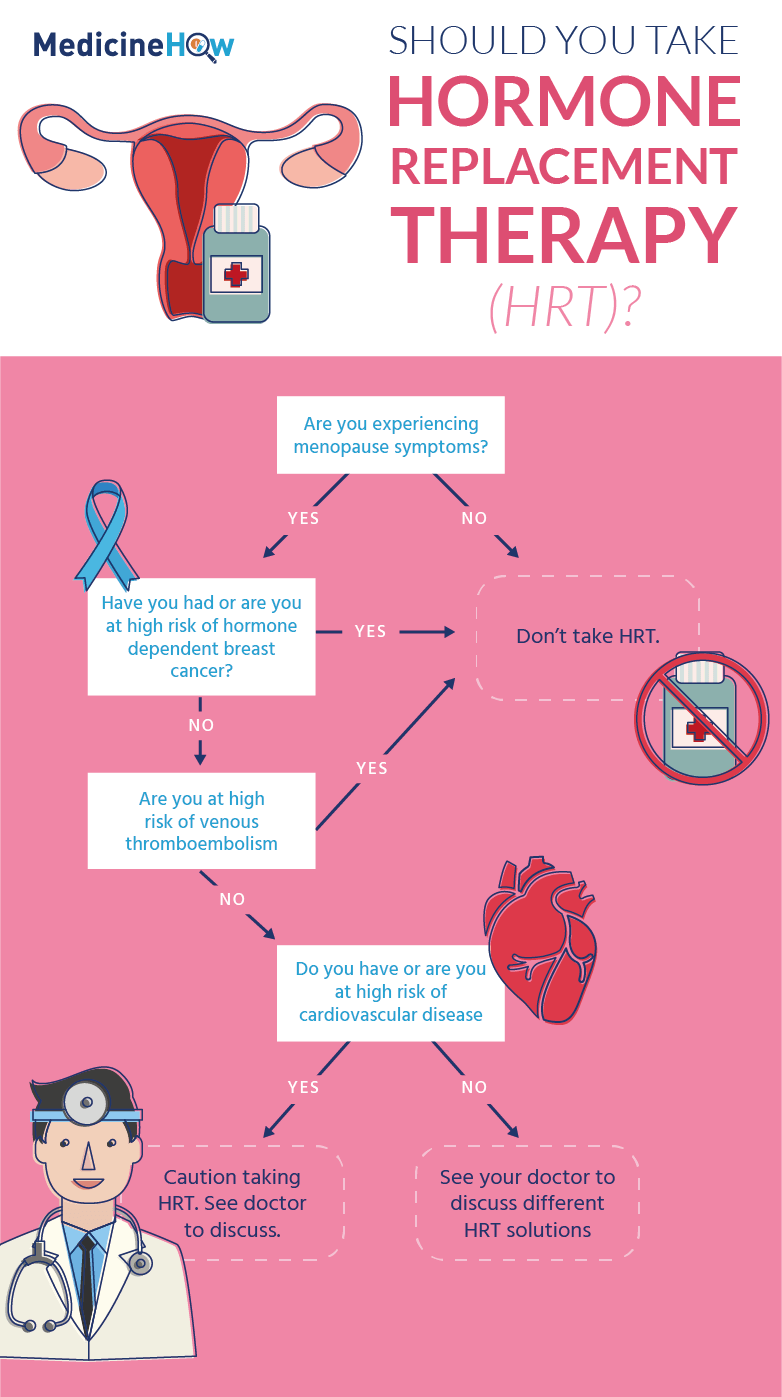
Weight gain at the menopause is related to age and lifestyle factors. An increase in body fat, especially around the abdomen, can occur during menopause because of hormonal changes, although exactly why this happens is not clear. Normal age-related decrease in muscle tissue, and a decrease in exercise levels, can also contribute to weight gain.
Most studies do not show a link between weight gain and HRT use. If a woman is prone to weight gain during her middle years, she will put on weight whether or not she uses HRT.
Some women may experience symptoms at the start of treatment, including bloating, fluid retention and breast fullness, which may be misinterpreted as weight gain. These symptoms usually disappear once the therapy doses are changed to suit the individual.
Recommended Reading: Estrace Weight Gain
What Questions Remain In This Area Of Research
The WHI trials were landmark studies that have transformed our understanding of the health effects of MHT. Its important to note that women who were enrolled in the WHI trials were, on average, 63 years old, although about 5,000 of them were under age 60, so the results of the study may also apply to younger women. In addition, the WHI trials tested single-dose strengths of one estrogen-only medication and one estrogen-plus-progestin medication .
Follow-up studies have expanded and refined the original findings of these two trials. But many questions remain to be answered:
- Are different forms of hormones, lower doses, different hormones, or different methods of administration safer or more effective than those tested in the WHI trials?
- Are the risks and benefits of MHT different for younger women than for those studied in the WHI trials?
- Is there an optimal age at which to initiate MHT or an optimal duration of therapy that maximizes benefits and minimizes risks?
How To Get Started On Hrt
Speak to a GP if youre interested in starting HRT.
You can usually begin HRT as soon as you start experiencing menopausal symptoms and will not usually need to have any tests first.
A GP can explain the different types of HRT available and help you choose one thats suitable for you.
Youll usually start with a low dose, which may be increased at a later stage. It may take a few weeks to feel the effects of treatment and there may be some side effects at first.
A GP will usually recommend trying treatment for 3 months to see if it helps. If it does not, they may suggest changing your dose, or changing the type of HRT youre taking.
Also Check: Does Blue Cross Blue Shield Cover Testosterone Therapy
Don’t Miss: How Long Does Olly Sleep Take To Work
Menopause Symptoms & Signs
Some of the symptoms of menopause can actually begin years before menstrual periods stop occurring. Doctors generally use the term “perimenopause” to refer to the time period beginning prior to the menopause up through the first year following menopause. Menopause itself is defined as having had 12 consecutive months without a menstrual period.
Menopause symptoms begin gradually while the ovaries are still functioning and a woman is still having menstrual periods. These symptoms can begin as early as the 4th decade of life and may persist for years until menopause has occurred. The symptoms occur early because the levels of hormones produced by the ovaries decline slowly over time, explaining why pregnancy is still possible, but less likely to occur, as a woman reaches her forties. The severity and duration of symptoms vary widely among individuals – some women may experience only minimal symptoms for a year or two, while others may experience at least some of the symptoms for several years.
While most women will experience a gradual transition to menopause with a slow onset of symptoms, some women will experience an early menopause that may bring on immediate symptoms, depending on the cause of the ovarian failure. One common cause of immediate symptoms is a “surgical menopause” following the surgical removal of functioning ovaries.
Menopause symptoms can be perceived as physical problems, emotional disturbances, or problems associated with sexual functioning.
Key Points: Coronary Artery Disease
-
1. In women aged less than 60 years and/or within 10 years of menopause with no evidence of cardiovascular disease, the initiation of hormone therapy could be expected to reduce the incidence of coronary heart disease and all-cause mortality.
-
2. The effect of hormone therapy on coronary heart disease may differ depending on the use of progestogen and the timing of initiation.
-
3. Currently, it is not recommended to initiate MHT solely for primary or secondary prevention of coronary heart disease.
Don’t Miss: Does Blue Cross Blue Shield Cover Testosterone Replacement Therapy
Information For Your Doctor To Read Includes Ams Information Sheets:
If you have any concerns or questions about options to manage your menopausal symptoms, visit your doctor or go to the Find an AMS Doctor service on the AMS website.
NOTE: Medical and scientific information provided and endorsed by the Australasian Menopause Society might not be relevant to an individuals personal circumstances and should always be discussed with their own healthcare provider. This Information Sheet may contain copyright or otherwise protected material. Reproduction of this Information Sheet by Australasian Menopause Society Members, other health professionals and their patients for clinical practice is permissible. Any other use of this information must be agreed to and approved by the Australasian Menopause Society.
If I Do Take Hrt How Can I Reduce My Risks
If you do decide to use HRT, there are ways to limit your risks. One approach is to keep your hormone use as low as possible. For example:
-
Use the lowest dose of estrogen that will provide you with relief.
-
If you only have vaginal symptoms, consider using a vaginal estrogen . Vaginal estrogen usually circulates throughout your body at a lower level.
-
Use HRT mindfully. Consider checking in with your healthcare provider every 3 to 6 months or at least annually to talk about your medication, and to re-evaluate your overall health. In some cases, your provider may recommend you taper off of HRT after 2 to 5 years to limit your risks, especially if you have been stable for years. They may also recommend lower doses of hormones as you get older.
If you are concerned about blood clots, you can also consider using a skin-based medication, like a:
-
Patch
-
Cream
-
Spray
These types of medication do not seem to have the same risks for serious blood clots that oral medications do. Skin-based and vaginal estrogen treatments may also have a lower risk for stroke than pills and tablets do.
Finally, lifestyle choices can help you stay healthy while on HRT. Consider:
-
Getting regular exercise
-
Maintaining a healthy weight
You May Like: Cost Of Estradiol
What Are The Types Of Hormone Therapy
There are two main types of hormone therapy :
- Estrogen Therapy: Estrogen is taken alone. Doctors most often prescribe a low dose of estrogen to be taken as a pill or patch every day. Estrogen may also be prescribed as a cream, vaginal ring, gel or spray. You should take the lowest dose of estrogen needed to relieve menopause symptoms and/or to prevent osteoporosis.
- Estrogen Progesterone/Progestin Hormone Therapy : Also called combination therapy, this form of HT combines doses of estrogen and progesterone .
How Is Menopause Diagnosed

Menopause is diagnosed starting with an assessment of a woman’s menstrual cycle history and a history of menopausal symptoms. In general, if a woman is over 45 years and presents with menopausal symptoms such as irregular menstrual periods, hot flashes, sleep problems, and mood changes, she would be considered in perimenopause and no diagnostic testing is needed.
Blood tests that may be indicated include:
For women 40 to 45 years who present with menopausal symptoms, blood tests to check for other conditions may include:
- Human chorionic gonadotropin to rule out possible pregnancy
- Prolactin to rule out hyperprolactinemia
- Thyroid stimulating hormone to rule out hyperthyroidism
Also Check: Estradiol Patch Price
What Is Considered Hormone Therapy Icd 10
Hormone replacement therapy ICD 10 is a medication that contains female hormones. You take the medication to replace the estrogen that your body stops making during menopause. Hormone therapy is most often used to treat common menopausal symptoms, including hot flashes and vaginal discomfort.
Leave us your review about this article!
| Submit your review |
Why Do People Need Hormone Replacement Therapy Icd 10
The issue of menopause ICD 10 is very popular in the world. Women from different countries give close heed to its effects and results. Therefore, it makes sense to clarify why it is needed.
Postmenopausal hormone replacement therapy ICD 10 is based on the treatment that involves drugs and devices that can increase the level of estrogen and progesterone. The insufficiency of these two hormones leads to discomfort and supporting diseases. Louise R. Newson asserts that more than 80% of women kept in secret their menopausal symptoms, and only 10% of British women underwent HRT in 2016.
Regarding the study published in the Scientific World Journal, private hospitals practice HRT 5.4 times more compared to public hospitals. Experts at university hospitals deal with hormonal imbalance ICD 10 12.3 times more than private and public hospitals. It proves that health providers practice more at universities trying new approaches and medications. The reasons for HRT can be different. The procedure involves specialists who examine a patient with the help of blood testing to see the level of the required hormone. Hormonal imbalance ICD 10 deals with disorders of the endocrine system that controls the production of hormones. HRT is popular among women who suffer from menopausal problems connected with the lack of estrogen or progesterone which decreases due to the aging process that affects the functionality of ovaries.
Recommended Reading: How Much Is Estrogen Pills
Key Points: Venous Thromboembolism
-
1. MHT increases the risk of venous thromboembolism. Particularly, the risk of VTE increases with age and increases in women initiating hormone therapy more than 10 years from menopausal onset.
-
2. The risk of venous thromboembolism increases in the first 1 to 2 years of MHT and decreases afterwards.
-
3. Estrogen therapy has a lower risk of venous thromboembolism than EPT, and if used in the early postmenopausal period, the risk of venous thromboembolism does not increase.
-
4. Oral estrogen therapy is banned for patients with anamnesis of venous thromboembolism, and they must use transdermal estrogen.
-
5. The occurrence of venous thromboembolism in Asian women is very low, and there has been no report of factor V Leiden mutation in South Korea.
Key Points: Mht For Women In Menopausal Transition
-
1. It is advised not to conduct a hormone test to diagnose menopause during menopausal transition.
-
2. Hormone therapy during menopausal transition should primarily be conducted based on the frequency and severity of symptoms, and lifestyle adjustments and use of adjuvant therapy could be partially effective.
-
3. EPT, low-dose COCs, and combination therapy of LNG-IUS with oral or percutaneous estrogen could be employed as individualized treatments depending on individual risk factors for the purpose of improving symptoms.
Also Check: Does Blue Cross Blue Shield Cover Low Testosterone
When Doctors Refuse To Administer Icd 10 Hormone Replacement Therapy
Menopause ICD 10 is not a universal approach. Moreover, it is not equally safe for everyone. There are certain circumstances when it is strictly forbidden for some groups of females. If they have definite health problems or take definite medications, it may provoke severe health problems. Besides, pregnant women should not pass Menopause ICD 10. Consequently, you must always consult a specialist in the field to discuss all the peculiarities and potential risks.A GP examines a patient and studies her medical history to make sure that she can take hormones. Pregnancy, breast cancer, womb cancer, ovarian cancer, hypertension, cardiovascular diseases connected with blood clots, liver disease, kidney dysfunction belong to the contradicting factors. A therapeutist usually asks questions about womens family medical history to find out whether a mother, a grandmother, or sisters have or had cancer of reproductive organs or mammary gland or problems with the heart or hypertension.
Always follow the instructions and prescriptions of your physician. Otherwise, you may sufficiently endanger your health. Do not undergo therapy at clinics and centers with a low reputation.
Actions For This Page
- Menopausal symptoms can be managed with education, lifestyle changes, support and hormone replacement therapy , also known as menopausal hormone therapy .
- In the early postmenopausal years, HRT is an effective therapy for menopausal symptoms. In most women with moderate to severe symptoms, the benefits outweigh the small increases in risk.
- The long-term use of HRT has some benefits, but also has some risks.
- The current role of HRT is for menopausal symptom relief, at the lowest effective dose and for the shortest duration required for the control of bothersome menopausal symptoms.
- The decision to use HRT, and for how long it should be used, must be based on individual assessment and needs.
Don’t Miss: Microgestin And Hair Loss
How Do I Know If Hormone Replacement Therapy Is Right For Me
Your doctor can help you weigh the pros and cons and suggest choices based on the severity of your symptoms and your medical history.
Here are some questions to ask:
- Based on my medical history, is there any reason I shouldnât use HRT?
- Do you think it could help my symptoms, especially hot flashes, sleep issues, and vaginal dryness?
- Are there other treatments I should consider?
- Do you think Iâll have side effects from HRT?
- Does my family medical history make me a good or bad candidate for HRT?
- What type of HRT might be best for me?
Show Sources
Menopausal Hormone Therapy And Cancer Risk
For decades, women have used hormone therapy to ease symptoms of menopause, such as hot flashes and sweating. This is called menopausal hormone therapy, and you may see it abbreviated as HT or MHT. You may also hear it described as hormone replacement therapy , postmenopausal hormone therapy , or postmenopausal hormones .
In the past, many doctors and their patients believed that MHT didnt just help with hot flashes and other symptoms it had important health benefits. But well-conducted studies have led many doctors to conclude that the risks of MHT often outweigh the benefits.
This information covers only how MHT can affect a womans risk of getting certain cancers. It does not cover other possible risks of MHT such as heart disease or stroke.
You can use this information when you talk to your doctor about whether MHT is right for you.
You May Like: Nugenix Estrogen Blocker