What Are The Risks Of Iud Birth Control
Overall, IUDs are a safe, effective form of birth control. Certain health conditions may increase the risk of IUD complications, including:
- Pelvic or other infections
- Uterine fibroids or tumors
Getting pregnant with an IUD is rare, but it can happen. You should call your doctor if you believe you may be pregnant at any time while you have an IUD.
British Columbia Specific Information
Birth control can help prevent pregnancy. There are many types of birth control available. Speak with your health care provider to help decide which type is right for you and your partner.
Hormone-based birth control contains hormones such as estrogen and progestin. Certain medications may make your hormone-based birth control not work properly or not at all. For more information, see HealthLinkBC File #91a Hormonal Contraception and using other medications at the same time.
Emergency contraception helps to prevent pregnancy after unprotected sex, or failed birth control. For more information about emergency contraception, see HealthLinkBC File #91b Emergency Contraception .
Birth control cannot prevent sexually transmitted infections , but using a condom will reduce your risk. For more information about birth control and sexual health, visit Options for Sexual Health and Smart Sex Resource. To learn more about STIs, see our HealthLinkBC Files – Sexually Transmitted Infections Series.
You may also call 8-1-1 to speak with a registered nurse or pharmacist. Our nurses are available anytime of the day, every day of the year. Our pharmacists are available every night from 5:00 p.m. to 9:00 a.m.
Which One Works Faster
IUDs are usually fitted during a period or within seven days of a period. This ensures a woman is not pregnant before the IUD is inserted. IUDs can be fitted at other times but a pregnancy test may be required beforehand.
ParaGard is effective immediately. It is also approved for use within 5 days of unplanned sexual intercourse as a form of emergency contraception.
Mirena is also effective immediately if fitted during the first seven days of menstruation, or if a reliable contraceptive method is being used however, your doctor may recommend you do not have intercourse or use tampons for up to 24 hours after insertion to minimize the risk of infection.
Neither device protects against sexually transmitted infections and all IUDs should only be inserted and removed by health care professionals experienced with the procedure.
Don’t Miss: Can Tubal Ligation Cause Early Menopause
How Do I Get A Copper Iud
Only a specially trained doctor or nurse can put in an IUD. You may need to make two visits.
- the doctor or nurse will ask questions about your health
- you might have a vaginal examination, a cervical screening test or a test for infection
- putting the IUD in takes about 10 minutes – you will be at the clinic for about 1 hour
- you may find it uncomfortable or painful and some women feel faint
- you can have a local anaesthetic
- some women have the IUD inserted under sedation – not all clinics provide this
After your copper IUD is put in:
- you may have cramps and bleeding or spotting in the first few days – you can take paracetamol or ibuprofen or use a heat pack. If cramps, spotting or pain last more than a few days, see your doctor
- avoid sex, tampons, swimming and baths for 2 days to reduce the risk of infection
- go back for a check-up 4 to 6 weeks after the IUD is put in
- check the IUD threads each month after your period to make sure the IUD is still in the right place – your doctor or nurse will show you how to do this
Things to remember with your copper IUD:
What Make The Copper And Hormonal Iuds Different

According to the experts that spoke to POPSUGAR, the ParaGard and the Mirena are both intrauterine contraceptive devices that differ mainly in their contraceptive agents. The “ParaGard is a nonhormonal, long-acting reversible contraception , and the Mirena is a hormonal LARC,” said board-Certified OBGYN Dr. Kameelah Phillips, MD IBCLC. According to Planned Parenthood, LARCs prevent unwanted pregnancy up to 20 times more effectively than birth control pills, patches, and vaginal rings. “LARCs are the most effective forms of reversible contraception,” adds board-certified OBGYN Dr. Kiarra King, MD FACOG.
While the ParaGard’s contraceptive agent is the thin copper coil wrapped around the device, the Mirena prevents pregnancy by emitting a small amount of the hormone progestin slowly overtime. According to Dr. Phillips, “both LARCs offer contraception for several years. The ParaGard for up to 10 years, and the Mirena for up to five years.”
Read Also: Does Tubal Ligation Cause Early Menopause
Why Can The Paragard Be Left In Longer Than The Mirena
According to our experts, the main reason why the ParaGard and Mirena differ in duration of effectiveness is because of their contraceptive ingredients. “The Mirena has the hormone essentially infused into the device which is released daily, but will eventually run out,” said Dr. King, explaining this is why it’s FDA-approved for a maximum of five years after its insertion. The action of the ParaGard’s copper coil, on the other hand, “lasts longer than the slow release progesterone that is present in the Mirena,” according to Dr. Phillips.
Iuds: How Do They Work
“IUDs are a good option for women because they are long-acting and reversible, and some types offer benefits beyond contraception,” such as helping to reduce heavy menstrual bleeding, says Christopher Destephano, MD, MPH, a gynecologist at the Mayo Clinic in Jacksonville, Florida.
IUDs are a type of contraception known as long-acting reversible contraception, or LARC. Another LARC is a contraceptive implant such as Nexplanon or Implanon. In recent years, LARCs have become more popular in the United States as a birth control method. The increasing interest in the IUD, a relatively expensive contraceptive option, is attributed, in part, to the passing of the Affordable Care Act in 2010, which made most health insurers cover at least one form of the IUD. What’s more, one study published in JAMA Internal Medicine in February 2019 found insertion rates jumped 21 percent in the 30 days after the 2016 election, probably because of concerns that the new administration would eliminate the existing mandate for free or inexpensive birth control.
You May Like: Nugenix Estro-regulator Reviews
How Does The Hormonal Iud Work
Once placed in the uterus, this type of IUD slowly releases small amounts of the hormone Levonorgestrel to prevent the sperm from reaching the egg.
Similar to hormonal birth control pills, the hormonal IUD can also prevent ovulation or the release of an egg from the ovary.
The hormones also thicken the cervical mucus to prevent sperm from swimming into the egg , they dilute the uterine lining to prevent implantation of the fertilized egg.
In addition to preventing pregnancy, the hormonal IUD can also . The Mirena device can cause menstruation to be absent .
Should I Be Worried If My Period Changes After Iud Insertion
According to Dr. King, “it is very common for people to notice changes in menstrual patterns and flow after an IUD insertion.” She added that “generally, with a hormonal device, bleeding may be irregular initially after insertion, but will often become lighter as time goes on, simply due to the effect of the hormone on the uterine lining.” On the other hand, since periods can become heavier with the ParaGard, “it is important to monitor your periods if they become heavier with ParaGard,” explained Dr. Phillips, as “heavier periods over time can cause anemia.”
Read Also: Can Having Your Tubes Tied Cause Hormonal Imbalance
Other Advantages Of The Hormonal Iud
Also, the hormonal IUD:
- Reduces heavy menstrual bleeding by an average of 90% after the first few months of use.footnote 4
- Reduces menstrual bleeding and cramps and, in many women, eventually causes menstrual periods to stop altogether. In this case, not menstruating is not harmful.
- May effectively relieve endometriosis and is less likely to cause side effects than high-dose progestin.footnote 5
- Reduces the risk of ectopic pregnancy.
- Does not cause weight gain.
Which Is Less Likely To Cause Bleeding
Bleeding problems, including heavy bleeding, spotting between periods and cramping are common for the first 2-3 months after ParaGard insertion. On average, ParaGard increases the duration and amount of menstrual bleeding resulting in an approximately 50% greater blood loss. Women should talk to their doctor if these changes persist or they have any concerns. Ongoing bleeding problems are a common reason women request removal of ParaGard.
Levonorgestrel can cause changes in a woman’s bleeding patterns. Spotting may occur for the first few months and subsequent periods are likely to be lighter and shorter. 20% of women experience a complete cessation of periods within a year of starting Mirena. Mirena is also the only IUD approved to treat heavy periods, and it is very effective for this, with an 80% reduction in bleeding after three months and a 90% reduction in bleeding after 6 months. This is attributable to the continual release of low-dose levonorgestrel contained in Mirena that prevents the endometrial lining from thickening up, which is what happens during a normal menstrual cycle. Mirena represents a much more acceptable treatment for heavy menstrual bleeding than hysterectomy.
Also Check: Breakthrough Bleeding On Bioidentical Hormones
How Should Paragard Be Taken
ParaGard is placed in your uterus during an office visit. Your healthcare provider first examines you to find the position of your uterus. Next, he or she will cleanse your vagina and cervix, measure your uterus, and then slide a plastic tube containing ParaGard into your uterus. The tube is removed, leaving ParaGard inside your uterus. Two white threads extend into your vagina. The threads are trimmed so they are just long enough for you to feel with your fingers when doing a self-check. As ParaGard goes in, you may feel cramping or pinching. Some women feel faint, nauseated, or dizzy for a few minutes afterwards. Your healthcare provider may ask you to lie down for a while and toget up slowly.
No Birth Control Is Perfect
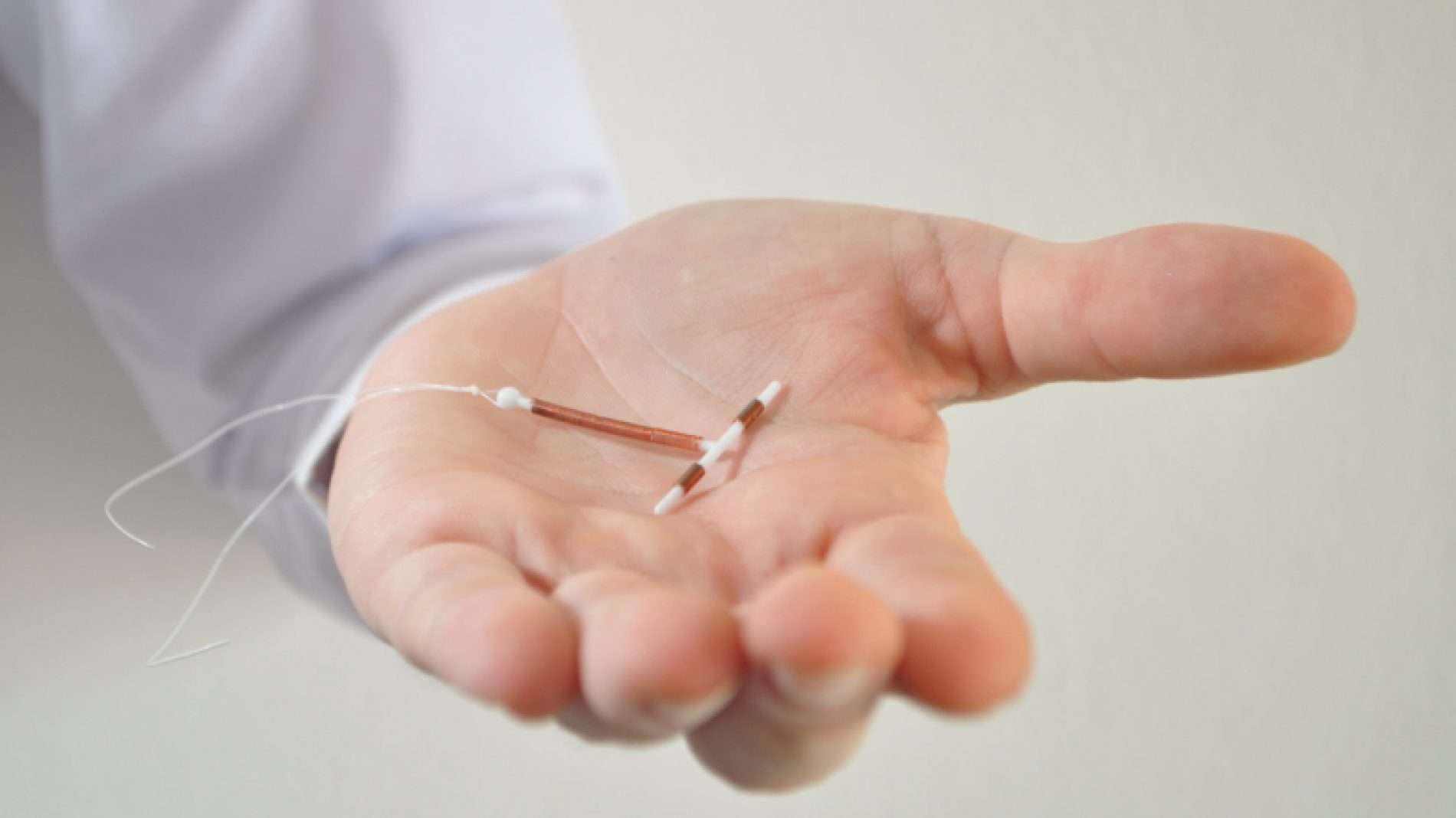
General warnings: There is a 1 percent chance that the insertion process will cause uterine perforation, which can lead to serious infections if left untreated. IUD expulsion, or when the IUD gets pushed out of the uterus, can happen, though not frequently â about .05 percent-8 percent of women who get the IUD deal with this problem. Like all forms of birth control, it can fail or cause health problems. BEING FERTILE IS A CHORE, Y’ALL.
The copper IUD is obviously dangerous for women with a copper sensitivity. It can also make periods heavier and cramps worse. If you have the option to use Mirena or Skyla, and you also already have painful periods, then the ParaGard may not be ideal for you. But you might love the hormonal ones. Remember, those ones make your period lighter.
I spoke to one woman who has Mirena, and she began suffering from yeast infections on a regular basis after its insertion. That does not happen to all women with IUDs, but it’s a frustrating side effect for her that you may want to bring up with your doctor. Still, even she plans to keep her IUD because of all of its positives.
An âadjustment periodâ follows the insertion, wherein your body gets used to the foreign object. For a lot of women, this means Advil, Tylenol, heating pads, and sleep to battle the headaches, cramps, and body aches. Unfortunately, the adjustment period can last a bit over a month, but the eventual peace of mind is so worth it for many women.
Recommended Reading: Can Having Your Tubes Tied Cause Hormonal Imbalance
Mirena Vs Copper Coil: Which One Is Best
Once you have decided what birth control product you would like to try, choosing the brand and type of that particular contraceptive is a decision in itself.
To help you make the best choice for you, and hopefully without having to conduct so much trial and error, The Lowdown lays out the ins and the outs of contraceptives.
This week, we bring you a comparison between the Mirena coil and the Copper coil.
The Benefits Of Hormonal Iuds: Mirena & Skyla
The two hormonal IUDs are called Mirena and Skyla, ’cause us gals love birth control with fun names! That being said, both work by âreleasing a low amount of the progestin, levonorgestrel,â and the said hormone thickens mucous in the cervix and thins the uterine lining, making it harder for sperm to enter. Skyla is a bit smaller than Mirena, releasing 14 mcg of progestin daily, as opposed to 20 mcg. Both still release less hormones than other birth control options. Moreover, because the IUD is taking up residence in your uterus, fertilized eggs cannot easily implant themselves. It’s like a uterus fort! Mirena is 99.8 effective at preventing pregnancy and Skyla is 99.1 percent effective at preventing pregnancy.Some of the hormonal IUD benefits, aside from the fact that you will not give birth when it’s not part of your life plan, include lighter periods â if any periods. Some women have also reported experiencing less painful cramps, or they report less full-body aches, and instead have cramps in more focused areas. They can reduce endometriosis pain and lessen endometrial cancer risks. Also, the thickening of cervical mucous lessens the risk of pelvic inflammatory disease by making it harder for STIs to enter. But again, use a condom for protection against STIs and HIV.
You May Like: Melatonin And Unisom Together
Nonhormonal Or Copper Iuds
Copper IUDs do not use hormones. Instead, the copper damages sperm to prevent it from getting to the egg. It also creates an immune response that stops the development of healthy eggs and destroys any eggs that do develop.
In the United States, the brand name of the copper IUD is ParaGard.
ParaGard IUDs begin working immediately, so doctors may choose them when emergency contraception is necessary. The copper IUD can prevent pregnancy for up to 10 years and possibly longer.
As with any birth control, the IUD offers benefits but also carries risks. People may wish to talk to a doctor about their medical history and any plans regarding future pregnancy before deciding which IUD is right for them.
The pros and cons of different types of IUD include:
How Hormones Work In The Ius
Unlike with the contraceptive pill or other forms of hormonal contraception, the hormones in the IUS are local, which means they only work within the area of your uterus. This means the hormones are less likely to have an impact on your mood or cause other physical symptoms that might occur with other hormonal contraceptives.
You May Like: Does Kaiser Cover Hormone Replacement Therapy
Are There Any Other Potential Side Effects We Should Know About Before Getting An Iud
In addition to the potential side effects for each listed above, Dr. Phillips shared that “all IUDs carry the risk of making a small hole in the uterus and/or getting stuck in the uterus. The risk is very small,” Dr. Phillips assured us, but nonetheless, it is important information to know when deciding which birth control option is best for you.
Does Not Prevent Sexually Transmitted Diseases
Furthermore, the IUD only prevents pregnancy, not protecting the body against sexually transmitted diseases. Therefore, when using an IUD, it is recommended to use barrier contraceptive methods such as condoms, which protect against diseases such as AIDS or gonorrhea , for example.
The hormonal IUD makes menstrual cycles lighter, with less colic, slowing or even zeroing menstrual flow . The copper IUD can cause an increase in menstrual flow and the woman may experience more cramps than usual.
Don’t Miss: Can Having Your Tubes Tied Cause Hormonal Imbalance
How About The Non
The Paragard non-hormonal IUD prevents pregnancy thanks to a tiny copper filament wrapped around the T. Paragard contains no hormones of any kindits the only super-effective non-hormonal birth control method around . Paragard also works as highly effective emergency contraception, so if youre considering an IUD and have had unprotected penis-in-vagina sex in the last 5 days but dont want to be pregnant, that could be another point in its favor.
Most people who use Paragard have heavier, longer, or crampier periods, especially for the first few months. After 6 months, many Paragard users periods return to normal. If you already have really heavy or uncomfortable periods, or you are anemic , you might prefer a hormonal IUD.
The bottom line? IUDs are safe, effective, and totally reversible. Whichever IUD you and your provider decide is best for you, we all win with more long-lasting, low-maintenance birth control options available.
Sara Kennedy, MD, MPH, is an Obstetrician/Gynecologist in Oakland, California. Originally from Pennsylvania, Sara has studied and lived around the world, including a residency at Northwestern University in Chicago and a masters degree in Australia, where she met her husband! Sara is passionate about womens health, particularly helping women in vulnerable situations obtain the knowledge and resources they need in order to control their reproductive health.
What Is Good About The Iud
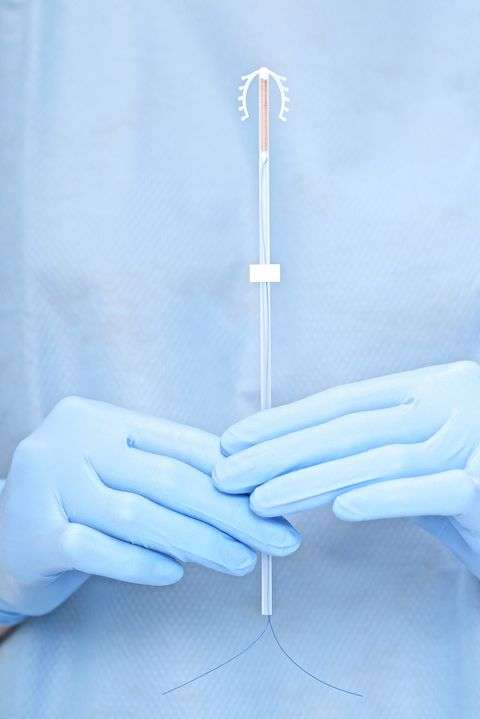
- It is an extremely effective method of contraception.
- Once inserted you will only need to check the string each month.
- It can last for 5 10 years .
- You can use it while breastfeeding.
- No medications stop it from working.
- It can be taken out at any time by a trained doctor or nurse.
- Once removed your fertility quickly returns to what is normal for you.
- It is another contraceptive option if you have difficulty taking the hormone oestrogen. The Pill and vaginal ring contain oestrogen and progestogen.
Don’t Miss: Can Having Your Tubes Tied Cause Hormonal Imbalance