Less Common Types Of Hormone Therapy
Some other types of hormone therapy that were used more often in the past, but are rarely given now include:
- Megestrol acetate , a progesterone-like drug
- Androgens , like testosterone
These might be options if other forms of hormone therapy are no longer working, but they can often cause side effects.
What Are The Symptoms
Many women donât have any symptoms of breast cancer when they get a diagnosis. Instead, doctors find it during a routine mammogram screening.
HR-positive breast cancer has the same symptoms as other types of breast cancer. Some of the more common symptoms include:
- A new lump in your breast
- Swelling of part or all of your breast
- Pain in your breast or nipple
- Changes in the skin over your breast
- Swollen lymph nodes, which may feel like lumps under your arm or near your collarbone
When Is Hormone Therapy Used For Breast Cancer
Hormone therapy is often used after surgery to help reduce the risk of the cancer coming back. Sometimes it is started before surgery .
It is usually taken for at least 5 years. Treatment longer than 5 years might be offered to women whose cancers have a higher chance of coming back. A test called the Breast Cancer Index might be used to help decide if a woman will benefit from more than 5 years of hormone therapy.
Hormone therapy can also be used to treat cancer that has come back after treatment or that has spread to other parts of the body.
Recommended Reading: Is Hormonal Breast Cancer Hereditary
Treatment Tailoring In Hormone
RT-PCR, reverse transcriptase-PCR. Modified from Sotiriou & Pusztai .
One of such tools, the Oncotype DX, merits to be addressed in more details . This test was developed to answer the following question Is it possible to identify a woman with hormone receptor-positive, lymph node-negative breast cancer, for whom it may be necessary something more than just tamoxifen alone? Among the 16 genes that the Oncotype DX analyzes, some are related to the ER , other related to cell proliferation , and other, like HER2, which are not functionally related. The relative expression of these genes compared with that of five reference genes whose expression does not correlate with tumor aggressiveness is combined by a mathematical formula that results in a continuous score ) that is directly proportional to the risk of metastatic relapse. The RS has been into divided into three risk categories by cutoffs that were established studying the clinical outcome of women enrolled in the tamoxifen arm of the NSABP B-20 clinical trial . The low-risk group has been defined by a RS< 18, the intermediate by a RS between 18 and 30, and the high risk by a RS> 30.
| 28 | 32 |
RS, recurrence score NSABP, national surgical adjuvant breast and bowel project ECOG, eastern cooperative oncology group SWOG, south western oncology group.
Side Effects Of Tamoxifen And Toremifene
The most common side effects of tamoxifen and toremifene are:
- Vaginal dryness or discharge
- Changes in the menstrual cycle
When tamoxifen treatment starts, a small number of women with cancer that has spread to the bones might have a tumor flare which can cause bone pain. This usually decreases quickly, but in some rare cases a woman may also develop a high calcium level in the blood that is hard to control. If this happens, the treatment may need to be stopped for a time.
Rare, but more serious side effects are also possible:
Recommended Reading: How To Fix My Hormones
Role Of Adjuvant Chemotherapy: Implications And Limitations Of The Metanalytic Approach
Metanalyses of randomized trials, especially those based on individual patient data, provide strong evidence of superiority of a treatment compared with another. However, it must be noted that this approach calculates average treatment-related effects and does not take into account the differential effect that the treatment under consideration has on biologically diverse subsets of tumors. Thus, treatment paradigms based on metanalyses can be the subject of criticism when it comes to their application in the clinical practice.
The latest fully published metanalysis of the EBCGTG suggested that six cycles of an anthracycline-based regimen like FAC or FEC should be considered the adjuvant chemotherapy treatment of choice in absence of medical contraindications . Rephrasing this concept, one regimen fits all . The alternative CMF-like regimens , which resulted inferior in terms of efficacy according to the comparisons made in the metanalysis, should be considered suboptimal because lesser efficacy impairs the therapeutic ratio, even in the presence of moderate reduction in the overall toxicities. Furthermore, the same paper consolidated two concepts that had already emerged in previous analyses:
In women with hormone receptor-positive breast cancer who are taking also tamoxifen, the benefits of endocrine therapy and chemotherapy are not mutually exclusive and, rather, tend to add each other .
Selective Estrogen Receptor Response Modulators
Selective estrogen receptor response modulators attach to and block estrogen receptors in breast cells. This stops the estrogen from signaling to the cells to grow.
Examples of SERMs include:
- toremifene for people with advanced ER-positive breast cancer after menopause
A doctor may prescribe one of these drugs with another medication.
Side effects
Possible adverse effects of SERMs include:
- changes in mood
- vaginal dryness or unusual discharge
Less commonly, SERMs may increase the risk of:
from the age of 5074. Those aged 4049 years should ask their doctor about whether screening is a good idea.
Other organizations have different recommendations. For example, the ACS recommends annual breast screenings for females aged 4554 years .
However, each persons situation is different. A doctor may recommend a different screening schedule for someone with a higher risk of breast cancer.
The outlook for people with ER-positive breast cancer tends to be good, especially when a doctor diagnoses it early.
A person with an early diagnosis of any type of breast cancer has a 99% chance of living for at least another 5 years, and often longer, the ACS reports.
However, if the cancer has spread to other organs, the chance of surviving for at least another 5 years is 29%, it notes.
Taking these steps may ultimately lead to a better outlook if a person develops breast cancer:
Don’t Miss: Does Hormone Therapy For Breast Cancer Cause Hair Loss
What Happens During Er/pr Testing
Your provider will need to take a sample of breast tissue in a procedure called a breast biopsy. There are three main types of breast biopsies:
- Fine needle aspiration biopsy, which uses a very thin needle to remove a sample of breast cells or fluid
- Core needle biopsy, which uses a larger needle to remove a sample
- Surgical biopsy, which removes a sample in a minor, outpatient procedure
Fine needle aspiration and core needle biopsies usually include the following steps:
- You will lay on your side or sit on an exam table.
- A health care provider will clean the biopsy site and inject it with an anesthetic, so you won’t feel any pain during the procedure.
- Once the area is numb, the provider will insert either a fine aspiration needle or core biopsy needle into the biopsy site and remove a sample of tissue or fluid.
- You may feel a little pressure when the sample is withdrawn.
- Pressure will be applied to the biopsy site until the bleeding stops.
- Your provider will apply a sterile bandage at the biopsy site.
In a surgical biopsy, a surgeon will make a small cut in your skin to remove all or part of a breast lump. A surgical biopsy is sometimes done if the lump can’t be reached with a needle biopsy. Surgical biopsies usually include the following steps.
Role Of Hormones In The Body
Our bodies naturally make hormones, including estrogen and progesterone.
Estrogen has multiple roles. It helps sex organs develop, makes pregnancy possible, strengthens bones, and more.
As you get older, the level of estrogen in your body changes.
- In women who have periods, the ovaries make most of the bodys estrogen. Estrogen levels in premenopausal women are usually high.
- In perimenopause, the ovaries slow down and make less estrogen. But it is still possible to have menstrual periods, even when the ovaries are working more slowly. Periods may sometimes be irregular. This in-between time happens several years before .
- In menopause, the ovaries gradually stop making estrogen. Periods become irregular and then stop altogether.
- Post-menopausal means a woman has not had any menstrual periods for 12 months in a row and blood work demonstrates hormonal levels are in post-menopausal range.
After menopause, the ovaries no longer make , the most active form of estrogen. But a womans body still makes estrone, another form of estrogen, after menopause. Estrone is made when an enzyme called aromatase converts the male sex hormone androstenedione made in the adrenal glands, ovaries, and fat cells into estrogen. In men, androstenedione is made in the testes.
Also Check: Hormonal Acne After Birth Control
Testing For Hormone Receptor
After a breast cancer , the removed sample of breast is sent to a lab for testing. If the tissue is confirmed to have cancer cells, the tests help your care team learn more about the cancer and how to treat it. Your doctor will share the test results with you in a document called a pathology report.
One test performed on breast cancer cells is called an immunohistochemical staining , or IHC test. This test checks the hormone receptor status of the cancer cells. IHC tests show whether the cancer cells have estrogen receptors, progesterone receptors, or both.
Optimal Sequence Of Therapy
There are many options in the sequencing of therapy for endocrine receptor-positive, metastatic breast cancer in post-menopausal women. Although first-line treatment with a CDK/4/6 inhibition has significant improvement in PFS, the total PFS is similar regardless of the sequencing . Treatment decisions should be based on medical comorbidities, prior adjuvant therapies, and disease-free interval . First-line treatment with an aromatase inhibitor or fulvestrant are still viable options and offer a PFS of 14 and 16.6 months, respectively. Frontline use of the combination of a CDK4/6 inhibitor with an aromatase inhibitor, such as palbociclib/letrozole and ribociclib/letrozole, offer a greater than 24-month PFS. Subsequent-line therapies include the use of palbociclib or abemaciclib with fulvestrant, the combination of everolimus with exemestane, and single-agent abemaciclib. The use of PI3K-inhibitors both single-agent and in combination with fulvestrant are being studied for use in patients with endocrine-resistant disease. Immunotherapy and CAR-T therapy are also being explored as other options of treatment. The use of biomarkers, including ESR1 mutation, and genomic profiling may provide useful future tools to direct therapy.
Fig. 1
Progression-free survival using endocrine therapy. a The PFS when aromatase inhibitors are used first line. b The PFS with the use of front-line CDK4/6 inhibitors
You May Like: Will Low Estrogen Cause Hair Loss
What Are The Side Effects Of Hormone Therapy
The side effects of hormone therapy depend largely on the specific drug or the type of treatment . The benefits and harms of taking hormone therapy should be carefully weighed for each person. A common switching strategy used for adjuvant therapy, in which patients take tamoxifen for 2 or 3 years, followed by an aromatase inhibitor for 2 or 3 years, may yield the best balance of benefits and harms of these two types of hormone therapy .
Hot flashes, night sweats, and vaginal dryness are common side effects of all hormone therapies. Hormone therapy also may disrupt the menstrual cycle in premenopausal women.
Less common but serious side effects of hormone therapy drugs are listed below.
Tamoxifen
- breathing problems, including painful breathing, shortness of breath, and cough
- loss of appetite
How Do Hormone Therapies Work
Hormone therapies slow or stop the growth of hormone receptor-positive tumors by preventing the cancer cells from getting the hormones they need to grow.
They work in a few ways:
- Some hormone therapies, such as tamoxifen, attach to the hormone receptor in the cancer cell and block estrogen from attaching to the hormone receptor.
- Some hormone therapies, such as aromatase inhibitors and ovarian suppression, lower the level of estrogen in the body so the cancer cells cant get the estrogen they need to grow.
Also Check: Is Low Testosterone Really An Issue
How To Manage A Hormone Receptor
Several -approved treatments available for hormone receptor-positive breast cancer are effective at reducing the risk of breast cancer . Because of this, you may hear people say that hormone receptor-positive breast cancer is the best breast cancer to have. We know hearing others say these kinds of things can be difficult or angering having any kind of cancer is challenging. Remember that your experience with breast cancer is your own. Its OK to feel overwhelmed, scared, depressed, and angry, because we all handle emotional and physical treatment side effects differently.
It’s important after a cancer diagnosis to surround yourself with people you trust and who allow you space to experience your emotions as they come. Not everyone in your life will be able to do this, and that can feel isolating. Here are some strategies to help you navigate your emotions after diagnosis:
- Write your feelings a journal
- Talk to a trusted friend or family member
or anti-estrogen , only works in hormone receptor-positive cancers. Different hormonal therapies work in different ways. One way is to block the estrogen and progesterone that the cancer relies on to grow and survive. Another way is to decrease the amount of estrogen produced in the body. These treatments disrupt the growth signals sent by the hormone receptors to cancer cells.
Depending on the type, hormonal therapy works by:
When used as recommended, it can:
Learn more about Types of hormonal therapy.
Hormone Receptors & Receptor Tests
All breast cancers are examined under a microscope for biomarkers of estrogen and progesterone receptors. About 70% of breast cancers are hormone receptor-positive.
Your hormone receptor status should appear on your pathology report after biopsy or surgery. Receptors will be retested if you ever have a recurrence or metastases as well, as your status can change.
Hormones and receptors go together kind of like a lock and key. Receptors are proteins on the surface of breast cells, and when hormones bind to them, the receptors tell the cells to grow and divide. All breast cells have receptors, but they are found in much greater numbers on breast cancer cells that are considered positive.
A goal of treatment is to block the signal created when the hormones attach to receptors. Doing that requires one of two things:
Most of the time, breast cancers tend to be positive or negative for both estrogen and progesterone receptors. Now and then, one will be positive for estrogen but not progesterone. The treatment is the same either way.
You May Like: What Hormones Affect Hair Loss
Are There Any Risks To The Test
You may have a little bruising or bleeding at the biopsy site. Sometimes the site gets infected. If that happens, you will be treated with antibiotics. A surgical biopsy may cause some additional pain and discomfort. Your health care provider may recommend or prescribe medicine to help you feel better.
Clinicopathologic Characteristics Of The Study Population
The flowchart of selection process was shown in Supplementary Figure 1. A total of 203406 patients were included, including 133662 patients for ER+PR+HER2-, 16906 for ER+PR-HER2-, 1395 for ER-PR+HER2-, 21439 for ER-PR-HER2- and 15646 for ER+PR+HER2+, 5381 for ER+PR-HER2+, 537 for ER-PR+HER2+, and 8440 for ER-PR-HER2+. The median follow-up duration of the study population was 35 months . The clinicopathologic characteristics of each subtype were summarized in Table 1.
Table 1 Clinicopathologic characteristics of the study population .
Also Check: Bioidentical Hormone Replacement Therapy Men
Symptoms Of Metastatic Breast Cancer
You may know that a lump in the breast is the most common symptom of breast cancer most lumps arent cancerous but its not the only one. Others include breast swelling, breast or nipple pain, red or flaking skin on the breast, abnormal nipple discharge, and swollen lymph nodes under the arms or close to the collarbone.
Lymph node swelling may be a sign that breast cancer is no longer confined to the breast. Metastatic breast cancer can cause a variety of symptoms, including fatigue, nausea, vomiting, poor appetite, and weight loss. Other symptoms of metastatic breast cancer are specific to the site that the disease affects, according to ASCO.
- If breast cancer spreads to the bones, it can cause pain in the joints, neck, or back. You may also have a higher risk of fractures.
- Breast cancer that moves to the brain can lead to headaches, nausea, dizziness, and vision problems, among other symptoms.
- If breast cancer affects the liver, you may experience jaundice yellowing of the skin itchy skin, abdominal swelling, and nausea.
- Metastatic breast cancer in the lungs can cause respiratory symptoms, such as shortness of breath, difficulty breathing, and a persistent cough.
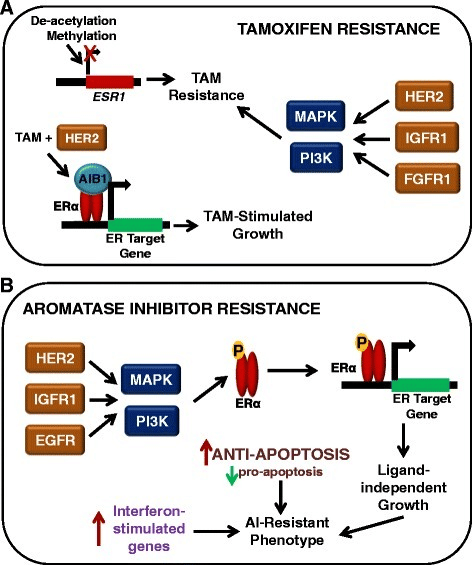
Resistance To Endocrine Therapy
Endocrine resistance is a major clinical problem encountered in the treatment of breast cancer. Endocrine resistance can be divided into two groups. Primary endocrine resistance is defined as relapse during the first 2 years of adjuvant endocrine therapy or progressive disease within the first 6 months of first-line endocrine therapy for metastatic breast cancer. Secondary resistance is defined as relapse while on adjuvant endocrine therapy but after the first 2 years of treatment, relapse within 12 months of completing adjuvant endocrine therapy, or progressive disease six or more months after starting endocrine therapy for metastatic breast cancer .
You May Like: Can You Have Too Much Melatonin