Mirena And Your Hormones
Weve talked before about issues with birth control pills, and Ill admit that while they are one of the oldest forms of hormonal birth control, they are probably my LEAST favourite.
In 2020 many more women are aware of the concerns with the pill, and they are unwilling to accept the common side effects the weight gain, breast tenderness, mood changes, zero libido, migraines, and more. So whats a woman to do?
Boosting Your Libido Naturally
If you’ve spoken with your healthcare provider and are still struggling with libido and your IUD, there are a few things you can do to treat it. The good news is, there are many natural and non-invasive remedies that you can use to get your libido back to where it should be.
Thereâs a good chance that thereâs nothing wrong with your body, but that there is something else that suppresses your sexual desire. If you suspect this is the case, we recommend you to take our assessment to find out what your situation is. Based on your answers, we will put together a relevant plan to start your journey towards better sexual wellbeing. If you want some more information on sex therapy, have a look at our complete guide on sex therapy.
Common Side Effects Of Kyleena Include:
-
Pain, bleeding or dizziness during and after placement. If these symptoms do not stop 30 minutes after placement, Kyleena may not have been placed correctly. Your healthcare professional will examine you to see if Kyleena needs to be removed or replaced.
-
Changes in bleeding. You may have bleeding and spotting between menstrual periods, especially during the first 36 months. Sometimes the bleeding is heavier than usual at first. However, the bleeding usually becomes lighter than usual and may be irregular. Call your healthcare professional if the bleeding remains heavier than usual or increases after it has been light for a while.
-
Missed menstrual periods. About 12 out of 100 women stop having periods after 1 year of Kyleena use. If you have any concerns that you may be pregnant while using Kyleena, do a urine pregnancy test and call your healthcare provider. If you do not have a period for 6 weeks during Kyleena use, call your healthcare provider. When Kyleena is removed, your menstrual periods should return.
-
Cysts on the ovary. About 22 out of 100 women using Kyleena develop a cyst on the ovary. These cysts usually disappear on their own in 2 to 3 months. However, cysts can cause pain and sometimes cysts will need surgery.
Also Check: Estradiol Patch Price
Can I Get Pregnant After The Iud Is Taken Out
Yes, you will be able to get pregnant as soon as the IUD is taken out.
Pregnancy is very rare with an IUD in place. If you do get pregnant with an IUD in, there is no extra risk for your baby, but there is a risk of complication in the pregnancy. If you think you might be pregnant, talk with your doctor as soon as possible. It is best to remove the IUD.
How Does Hormonal Iud Work

IUDs affect the way sperm move and survive in the uterus , stopping sperm from meeting and fertilising an egg. IUDs can also change the lining of the uterus, making it difficult for a fertilised egg to stick to the lining to start a pregnancy.
The hormonal IUDs also work by thickening the fluid around the cervix . This helps to prevent sperm from entering.
Sometimes the hormonal IUDs can also stop the ovaries from releasing an egg.
You May Like: What Causes Breakthrough Bleeding When On Bioidentical Hormones
What Are The Hormonal Intrauterine Devices
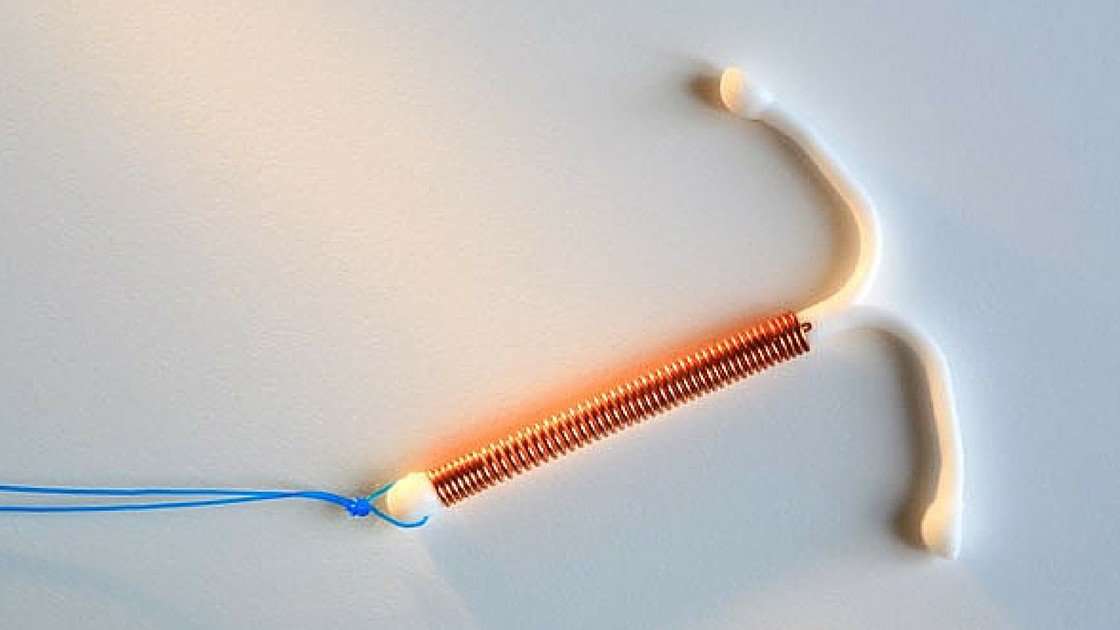
The hormonal IUDs are small T- shaped plastic devices that are inserted into the uterus . The hormonal IUDs contain progestogen. This is a synthetic version of the hormone progesterone made naturally by the ovaries. The hormonal IUDs have a coating that controls the slow release of progestogen into the uterus. There are two different hormonal IUDs available in Australia. They are sold as Mirena and Kyleena.
How Does The Mirena Work
The Mirena IUD, like all hormonal IUDs, contains a synthetic hormone called Levonorgestrel, a progestin, that it slowly releases in your body over time. While progestin sounds like progesterone, it is not, nor does it behave like progesterone in your body.
Instead, the progestin released thins the lining of your uterus, the endometrium, so a fertilized egg would be unable to implant. This is one way in which women have lighter or absent periods while using a hormonal IUD.
It is also designed to stop ovulation by suppressing the production of two brain hormonesFollicle Stimulating Hormone and Luteinizing Hormone . FSH and LH work together to mature an egg and trigger ovulation. They are also responsible for signaling the rise and fall of your hormones. It also thickens cervical secretions, making it difficult for sperm to make it to the egg in the event ovulation does occur.
Recommended Reading: Can Getting Your Tubes Tied Cause Early Menopause
You Might Have Irregular Spotting For A Few Months
Your uterus needs a minute to get used to the small T-shaped device that was just inserted into it. That means you’ll probably find some weird stains of blood on your panties at strange times of the month. Spotting is a super normal side effect of having an IUD inserted, and it likely lasts for the first few months of having one, so don’t panic and convince yourself that something is wrong ââ¬â unless, you know, you really feel like there is.
What Are The Advantages
- Long acting it lasts for between 3 and 10 years depending on the type of IUD
- Reversible you can choose to have it taken out at any time. After that, you will be able to get pregnant
- 99% effective it works very well
- You dont need to think about contraception every day
- Does not affect breastfeeding
- Does not get in the way of sex
- The copper IUD does not contain any hormones
- The copper IUD can also be used as emergency contraception
- The hormonal IUD has a very small amount of hormones and most people have no side effects from this
- The Mirena can help with period bleeding and pain, and most people will have light bleeding or no periods at all.
Studies show that IUDs do not cause pimples, headaches, sore breasts, nausea, mood changes, loss of sex drive or weight gain. There is no evidence of an extra risk of cancer.
Recommended Reading: How To Get Estrogen Mtf
What If I Am Using The Hormonal Iud And I Want To Become Pregnant
The hormonal IUD can be removed at any time by a trained doctor or a nurse. Your fertility will quickly return to what is normal for you.
If you are using the internet for information, only use reliable and reputable websites, such as the ones provided above.
DisclaimerThis website and any related materials are for general information purposes only and should not be relied on as medical or other professional advice. You should seek specific medical or professional advice for your individual circumstances.
The copyright for material on this website is owned by Family Planning Victoria and is subject to the Copyright Act 1968. We permit you to reproduce or communicate our copyright material if you are a not-for-profit educational organisation, for the purpose of providing the information to your students provided that you include any disclaimers associated with that material. Any other reproduction or communication of our material requires our prior consent, via our consent form which you can complete and submit.
30 August 2021
Family Planning Victoria acknowledges the Aboriginal and Torres Strait Islander people as the Traditional Owners of the land on which our offices stand and in the regions in which we provide our services. We pay our respects to Elders past, present and future.
How Is Mirena Used
The Mirena IUD is inserted through the vagina and placed into the uterus by a doctor.
You may feel pain or dizziness during insertion of the IUD, and you may have minor vaginal bleeding. Tell your doctor if these symptoms last longer than 30 minutes.
The Mirena IUD should not interfere with sexual intercourse, wearing a tampon or menstrual cup, or using other vaginal medications.
Your doctor should check the IUD after a few weeks to make sure it is still in place. You will also need annual pelvic exams and Pap smears.
You may have irregular periods for 3 to 6 months. Your flow may be lighter or heavier, and your periods may stop after several months. Tell your doctor if you do not have a period for 6 weeks or if you think you might be pregnant.
The Mirena IUD may come out by itself. After each menstrual period, make sure you can still feel the removal strings at the opening of your cervix.
If you need to have an MRI , tell your caregivers ahead of time that you have a Mirena IUD in place.
Your IUD may be removed at any time you decide to stop using birth control. The Mirena IUD must be removed at the end of the 6-year wearing time. Your doctor can insert a new device if you wish to continue using this form of birth control. Only your doctor should remove the IUD. Do not attempt to remove the device yourself.
If you decide to use a different method of birth control, you may need to start using it a week before your IUD is removed.
Also Check: What Causes Breakthrough Bleeding When On Bioidentical Hormones
Other Possible Side Effects Of Hormonal Iuds
Aside from the possible connection between IUDs and anxiety, there are other side effects from IUDs that can range from mild to severe. Most women feel a small, sharp pain when the IUD is put in and cramping or lower back aches for several days afterward. You may notice spotting more than usual between periods, irregular periods, or heavier periods and more severe cramps.
Most women feel a small, sharp pain when the IUD is put in and cramping or lower back aches for several days afterward.
Over-the-counter pain medication can help with the initial pain of having your IUD implanted and the cramping associated with your period. However, if the bleeding is unusually heavy and the cramping doesnt go away, see your doctor.
Other possible adverse effects of hormonal IUDs are amenorrhea , pelvic inflammatory disease, increased risks of ectopic pregnancy, and ovarian cysts.
Mirena As Contraception During Perimenopause
Anyone who has been using birth control to prevent pregnancy should continue to do so until they enter menopause.
While fertility typically starts to decline in a womanâs mid-30s, it is possible for some women to get pregnant into their 50s.
According to the standard definition, menopause has begun if 12 months have passed without a period. However, because the Mirena coil can stop periods from occurring, it is important to use another method of determining when menopause has begun.
A doctor may do a blood test to check for follicle-stimulating hormone and estrogen levels. During perimenopause, FSH levels typically rise as estrogen levels fall. The doctor may need to run the test more than once, since these levels can naturally fluctuate.
There is no set time to remove the Mirena coil, unless it expires.
Womenâs Health Concern recommend waiting for 1 year after the last period before stopping birth control.
Anyone who removes the Mirena coil before they enter menopause should switch to another form of birth control if they wish to prevent pregnancy.
Some people choose to wait until their coils expire, even after menopause has begun. A doctor can provide specific guidance.
Hormone replacement therapy can help alleviate some symptoms of menopause. It is not a form of birth control.
HRT injections, pills, or patches may ease some menopause symptoms, such as:
- night sweats
- lower bone density
- vaginal dryness
Read Also: Nugenix Estro Regulator Review
How Long Do Mirena Side Effects Last
In many cases, unwanted effects of the Mirena IUD are not long-term. According to Planned Parenthood, common side effects such as spotting between periods and cramping typically get better in 36 months.
Meanwhile, a person might want to have some side effects of Mirena, such as lighter periods or none at all. Research suggests that these are usually long-term changes for people who experience them while using the IUD.
Serious complications, such as PID, typically develop shortly after the person starts using the IUD often within the first month. These issues are uncommon.
Speak with a doctor about any severe or persistent symptoms that occur during Mirena IUD use.
The Mirena IUD releases the hormone levonorgestrel, a synthetic form of progesterone. Levonorgestrel works by thickening the cervical mucus and thinning the lining of the uterus, which prevents pregnancy from taking place. This synthetic hormone can also prevent ovulation, though it does not always have this effect.
The Mirena IUD has several key advantages. It:
However, there are some disadvantages, such as the:
- insertion procedure, which can be painful
- possibility of unwanted effects
- small risk of infection and other complications
- symptoms that may occur after the IUD is removed
It can take some time after a doctor removes the Mirena IUD for periods to return to normal. Also, some people experience a Mirena crash, which involves changes to their mood, sleep, weight, and skin health.
Who Can Get An Iud
Most people can use an IUD, including those who are young and those who have not had children.
Hormonal IUDs are a really good option if you have heavy or painful periods.
If you have an infection, you should get it treated before you get an IUD put in.
If you have heavy or painful periods you should not get a copper IUD because it might make them worse.
Don’t Miss: Does Blue Cross Blue Shield Cover Testosterone Therapy
Here Are A Few Reasons Why An Iud Could Be An Excellent Choice For You
What research has been done shows that hormonal IUDs fail just 0.2 percent of the time while the copper IUD fails 0.8 percent of the time. This means fewer than one out of 100 women will get pregnant each year when using an IUD. A lot of this comes down to the fact that IUDs are hard to mess up.
Birth control pills, on the other hand, have a failure rate that ranges from less than 1 percent with perfect use to 9 percent with typical use . So if youre worried about messing up your birth control, an IUD might be a good choice for you.
To put it simply, IUDs are one of the best methods of contraception that we have, Lauren Streicher, M.D., an associate professor of clinical obstetrics and gynecology at Northwestern University Feinberg School of Medicine, tells SELF. The only reversible contraceptive thats more effective than the IUD is the implant, which was found to have a 0.05 percent failure rate. That implant goes in your arm and can be used for up to three years.
Mirena and Kyleena are recommended for up to five years, Liletta is recommended for up to four years, and Skyla is recommended for up to three years. ParaGard, on the other hand, can be used up to 10 years. So if youre looking for long-term birth control , this could be a great option.
With methods like the pill, the ring, and the shot, you have to think about your birth control on a regular basis. But IUDs are different.
Cons Of The Hormonal Iud:
Hormonal IUDs can damage the vaginal microbiome and increase the risk of yeast infections and bacterial vaginosis.
Hormonal IUDs suppresses ovulation some of the time.
Hormonal IUDs can cause irregular bleeding and spotting during the first three to six months of use. After that, they may suppress bleeding entirely or permit a light natural menstrual period.
Insertion might be painful. But just to clarify: IUD is an in-office procedure that takes just a few minutesits not surgery. Youll probably be instructed to take a painkiller like ibuprofen to ease the cramping, or your doctor may decide to use a local anesthetic .
Hormonal IUDs can come out. The chance of expulsion is 5 percent but more likely immediately following childbirth and during breastfeeding.
Hormonal IUDs carry a small risk of uterine perforation, which could lead to surgery. The chance of perforation is 0.1 percent but more likely if during breastfeeding.
Hormonal IUDs can cause pelvic inflammatory disease but only during the first three weeks after insertion, and only if you have a pre-existing infection with gonorrhea or chlamydia.
Hormonal IUDs must be removed by a doctor. See my copper IUD post for more information about IUD removal.
Hormonal IUDs cannot protect against sexually transmitted infections.
You May Like: Nugenix Estro Regulator Side Effects
How Do I Use The Hormonal Iud
The hormonal IUD is inserted inside the uterus by a trained doctor or nurse. You can choose to have a local anaesthetic or sedation while it is inserted. The IUD insertion takes around 15 minutes but you will be in the clinic for an hour or more. See below for a video about IUDs and how to help prepare for and manage pain from an IUD insertion.
The IUD has a fine nylon string attached to it which comes out through the cervix . The string cannot be seen and it does not hang out of the vagina. If you feel high up inside your vagina, you can check that the string is there and know the IUD is still in place. It is good to do this every month. If the string feels like it is shorter or longer than normal or you cannot feel the string at all, the IUD may have shifted and you should see a doctor or nurse.