Definitions That May Help
Your doctor may use specific terms to let you know how your cancer is responding to hormone therapy or other treatments. They include:
- Castrate level: When the testicles are removed and testosterone levels plummet, this is referred to as the castrate level. Androgen levels that remain this low are most beneficial for reducing the impact of prostate cancer. Hormone therapy is designed to keep testosterone at castrate level.
- Castrate-sensitive prostate cancer : CSPC refers to prostate cancer that is being controlled successfully with testosterone at castrate level.
- Castrate-resistant prostate cancer : CRPC prostate cancer refers to cancer that is not successfully controlled, even though testosterone levels are at or below castrate level. CRPC may require additional medications, such as a CYP-17 inhibitor or one of the newer antiandrogens.
- Hormone-refractory prostate cancer : HRPC is prostate cancer that is no longer responsive to any type of hormone therapy, including newer medications.
Kinds Of Hormone Therapy
Hormone therapy is a category encompassing a number of treatments. In some conditions or diseases, certain hormones are prescribed in order to increase their levels. This is frequently referred to as hormone replacement therapy . Hormones can be natural or synthetic, meaning produced commercially . Patients who do not have prostate cancer but have symptoms from low testosterone levels, such as fatigue, may be prescribed testosterone as a type of HRT. In certain cases, patients with prostate cancer under control may receive this type of hormone therapy however, because of the risk of activating the cancer, some doctors advise against it. Male children or adults with hypogonadism are prescribed testosterone as HRT.
As mentioned previously, HT in prostate cancer aims to reduce production of the hormone testosterone, rather than increase it, thereby interfering with cancer cells ability to use it to grow.
The hormone therapies that have become standard prostate cancer treatments are the ones we discuss in detail in this guide. All decisions regarding these treatments should be carefully made by the patient and doctor together.
Hormonal Therapy With Radiotherapy
Hormonal therapy is often used to treat early and locally advanced prostate cancer. If you have low-risk early prostate cancer you do not usually need hormonal therapy.
Doctors often advise having hormonal therapy with radiotherapy , to make your treatment more effective. You may have hormonal therapy before, during and after radiotherapy. It can be given:
- a few months before radiotherapy, to shrink the cancer
- after radiotherapy, to reduce the chance of the cancer coming back .
Your doctor will talk to you about how long you take hormonal therapy for. They will also explain the possible side effects.
Recommended Reading: Ancient Nutrition Women’s Hormones Reviews
Table : Boosting The Effectiveness Of Radiation Therapy
A randomized controlled study involving 206 men with early-stage prostate cancer evaluated whether adding six months of hormone therapy to external-beam radiation treatment would boost both overall survival and disease-free survival . The results are given below. The same research group found, in an earlier study, that the addition of hormone therapy was of most benefit to men who were considered at moderate or high risk, based on their clinical profile.
Five-year follow-up 82% Source: Journal of the American Medical Association, 2004 292:8217. PMID: 15315996.
Combined with radiation therapy. A number of studies have shown that men with early-stage prostate cancer are more likely to be cured when hormone therapy is given in conjunction with radiation therapy . Even when the disease is regionally advanced, meaning that it has progressed to tissues immediately surrounding the prostate gland, neoadjuvant hormone therapy reduces risk of progression and relapse .
Why Does Hormone Therapy Stop Working
Over time, hormone therapy stops working for of prostate cancer.
With CRPC, prostate cancer continues to grow despite very low or undetectable androgen levels.
Hormone therapy may stop working if cancer cells develop a resistance to the treatment. ADT may destroy some cancer cells, while others may adapt and evolve to become resistant to those hormone therapies.
Experts are not entirely sure why prostate cancer cells eventually become resistant to hormone therapy.
Also Check: How Do Dermatologists Treat Hormonal Acne
How Is Prostate Cancer Diagnosed
Prostate cancer may be suspected based on your symptoms or the results of a screening test.
Screening is when your doctor looks for cancer before you have any symptoms. This can help find cancer at an early stage when it may be easier to treat. Two of the most frequently used screening tests used today include the digital rectal exam and the prostate-specific antigen test.
- A digital rectal exam is an exam of the rectum where the doctor inserts a lubricated, gloved finger into the lower part of the rectum to feel for lumps or enlargement in the prostate gland.
- A prostate-specific antigen is a blood test that measures levels of PSA in your blood. However, PSA is reasonably nonspecific and high levels may be associated with prostate cancer, prostatitis , or an enlarged prostate gland. Very high levels of PSA .
There is controversy over whether screening tests should be used at all. The USPSTF recommends men aged 55 to 69 have a discussion with their doctor about the pros and cons of PSA screening to determine if it is an appropriate preventive test for them. For men aged 70 and older, the USPSTF does not recommend PSA screening.
The American Cancer Society, recommends early-detection screening starting at age 40 or 45 if men are at high risk or age 50 in men at average risk.
In some cases, a prostate biopsy or imaging test like an ultrasound or magnetic resonance imaging may also be used to rule out cancer.
Early Versus Delayed Treatment
For men who need hormone therapy, such as men whose PSA levels are rising after surgery or radiation or men with advanced prostate cancer who dont yet have symptoms, its not always clear when it is best to start hormone treatment. Some doctors think that hormone therapy works better if its started as soon as possible, even if a man feels well and is not having any symptoms. Some studies have shown that hormone treatment may slow the disease down and perhaps even help men live longer.
But not all doctors agree with this approach. Some are waiting for more evidence of benefit. They feel that because of the side effects of hormone therapy and the chance that the cancer could become resistant to therapy sooner, treatment shouldnt be started until a man has symptoms from the cancer. This issue is being studied.
Don’t Miss: Online Doctor For Hormone Replacement Therapy
How Does Hormone Therapy Work
Hormone therapy for prostate cancer works by either preventing the body from making these androgens or by blocking their effects. Either way, the hormone levels drop, and the cancer’s growth slows.
“Testosterone and other hormones are like fertilizer for cancer cells,” Holden tells WebMD. “If you take them away, the cancer goes into shock, and some of the cells die.”
In 85% to 90% of cases of advanced prostate cancer, hormone therapy can shrink the tumor.
However, hormone therapy for prostate cancer doesn’t work forever. The problem is that not all cancer cells need hormones to grow. Over time, these cells that aren’t reliant on hormones will spread. If this happens, hormone therapy won’t help anymore, and your doctor will need to shift to a different treatment approach.
What Is The Most Effective Treatment For Prostate Cancer
The good news is that there are many effective treatments that can result in positive outcomes for prostate cancer patients. For example, for localized prostate cancer, external beam radiation therapy can have an up to 95% efficacy. Radical prostatectomy has also been found to achieve an over 90% efficacy against prostate cancer. The decision of which treatment plan or plans to follow is ultimately a personal decision that should be based on the recommendations of your doctor.
You May Like: What Is Cystic Hormonal Acne
Hormone Therapy And Prostate Cancer
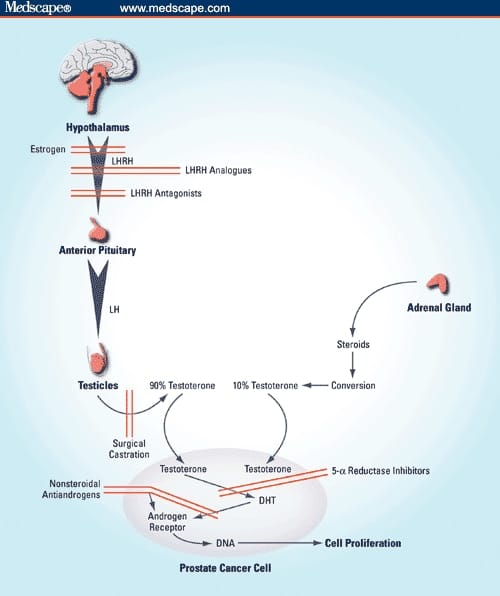
Prostate cancer is fueled by testosterone, a hormone produced in the testicles. The aim of HT is to interfere with either testosterone production or cancer cells’ ability to use testosterone. Medical evidence tells us that eliminating or substantially reducing testosterone production has a significant impact on controlling progression of the disease and may even halt progression. Testosterone is one of several hormones called androgens that are linked to sexual health and other processes in the body. This is why HT is often referred to as androgen deprivation therapy .
To be clear, this is not the “hormone therapy” of which you often hear. Women get “hormone therapy” to supplement waning estrogen levels, and older men without prostate cancer may get “hormone therapy” that administers additional testosterone. The “hormone therapy” we are talking about for men with prostate cancer is more accurately described as androgyn deprivation therapy . It is given to lower testosterone levels.
How Much Hormone Therapy Costs
The cost of hormone therapy depends on
- the types of hormone therapy you receive
- how long and how often you receive hormone therapy
- the part of the country where you live
Talk with your health insurance company about what services it will pay for. Most insurance plans pay for hormone therapy for their members. To learn more, talk with the business office where you go for treatment. You can also go to the National Cancer Institute database, Organizations that Offer Support Services and search financial assistance. Or call toll-free 1-800-4-CANCER to ask for help.
Also Check: Which Doctor To Consult For Female Hormonal Imbalance
Active Surveillance And Watchful Waiting
If prostate cancer is in an early stage, is growing slowly, and treating the cancer would cause more problems than the disease itself, a doctor may recommend active surveillance or watchful waiting.
Active surveillance. Prostate cancer treatments may seriously affect a person’s quality of life. These treatments can cause side effects, such as erectile dysfunction, which is when someone is unable to get and maintain an erection, and incontinence, which is when a person cannot control their urine flow or bowel function. In addition, many prostate cancers grow slowly and cause no symptoms or problems. For this reason, many people may consider delaying cancer treatment rather than starting treatment right away. This is called active surveillance. During active surveillance, the cancer is closely monitored for signs that it is worsening. If the cancer is found to be worsening, treatment will begin.
ASCO encourages the following testing schedule for active surveillance:
-
A PSA test every 3 to 6 months
-
A DRE at least once every year
-
Another prostate biopsy within 6 to 12 months, then a biopsy at least every 2 to 5 years
Treatment should begin if the results of the tests done during active surveillance show signs of the cancer becoming more aggressive or spreading, if the cancer causes pain, or if the cancer blocks the urinary tract.
Secondary Treatment Following Relapse

Hormone therapy may also be used as a secondary or salvage treatment when PSA levels rise following initial prostate cancer treatment, indicating the cancer has returned. This situation is known as biochemical recurrence. The salient points to keep in mind are that hormone therapy is most often used as a salvage treatment when PSA doubling time is less than six months, indicating that the cancer is aggressive or may have already metastasized.
Also Check: Will My Doctor Prescribe Testosterone
Current Treatment Strategies For Advanced Prostate Cancer
The current hormonal therapeutic armamentarium for advanced prostate cancer is informed by 2 broad approaches: inhibition of conversion of extragonadal precursor steroids to testosterone and DHT with abiraterone and direct blockade of the AR to prevent binding to its ligands, testosterone, and DHT with next-generation AR antagonists such as apalutamide, darolutamide, or enzalutamide .
Study Process And Results
Researchers working at 10 hospitals in Spain enrolled 355 men with newly diagnosed prostate cancer that was still confined to the prostate and seminal vesicles . The men were divided into two groups: one group received a short course of hormonal therapy lasting four months, and the other group was treated for a longer duration of 24 months. All the patients were also treated with high-dose radiation.
After 10 years, only men who had been diagnosed initially with high-risk prostate cancer benefited from the long-term treatments. Specifically, 67.2% of these men avoided subsequent increases in prostate-specific antigen that signified worsening cancer. By contrast, 53.7% of men with high-risk cancer who received four months of hormonal therapy avoided similar PSA increases. Importantly, 78.5% of high-risk men who had long-term hormonal therapy were still alive after 10 years, compared to 67% of high-risk men treated with hormonal therapy for four months.
Among men with intermediate-risk prostate cancer, the duration of hormonal therapy made little difference. Just four men with intermediate-risk cancer developed worsening cancer that had spread to other sites in the body. Two came from the short-term treatment group, and two from the group that received hormonal therapy for 24 months. And after 10 years, none of the intermediate-risk patients had died from prostate cancer, regardless of how long the hormonal therapy treatments lasted.
Recommended Reading: Diet Pills For Hormonal Weight Gain
When Hormone Therapy Is Indicated
HT can be administered before, during or after a localized treatment, such as radical prostatectomy, radiation, high-intensity focused ultrasound or cryotherapy. When given before a localized treatment, it is called neoadjuvant therapy. When given after localized treatment without evidence of prostate cancer recurrence, it is called adjuvant therapy. When HT is prescribed after localized treatment for a prostate cancer recurrence, it is called salvage therapy. If a patient’s PSA starts rising after a radical prostatectomy, HT is typically given in combination with radiation therapy. Treatment recommendations are based on each patient’s specific circumstances.
Sometimes we give neoadjuvant HT while the patient is deciding on his primary treatment or to reduce the tumor’s size before starting primary treatment. Neoadjuvant HT will usually slow or stop cancer growth for a period of time.
Many radiation oncologists use HT along with radiation treatment in the belief that HT weakens cancer cells so that they’re more susceptible to destruction by the radiation. Clinical studies have suggested a synergy between radiation therapy and hormone therapy meaning they work better together. Clinical trials have shown improved outcomes for patients who receive combined therapy.
How Does Hormone Therapy Work Against Prostate Cancer
Early in their development, prostate cancers need androgens to grow. Hormone therapies, which are treatments that decrease androgen levels or block androgen action, can inhibit the growth of such prostate cancers, which are therefore called castration sensitive, androgen dependent, or androgen sensitive.
Most prostate cancers eventually stop responding to hormone therapy and become castration resistant. That is, they continue to grow even when androgen levels in the body are extremely low or undetectable. In the past, these tumors were also called hormone resistant, androgen independent, or hormone refractory however, these terms are rarely used now because the tumors are not truly independent of androgens for their growth. In fact, some newer hormone therapies have become available that can be used to treat tumors that have become castration resistant.
Read Also: How To Know My Hormone Type
Nonmetastatic Crpc As An Evolving Clinical State
Interest has grown in the treatment of nonmetastatic castration-resistant prostate , a clinical state defined by rising PSA as evidence of progression despite castrate levels of testosterone and lack of radiologic evidence of metastases upon standard-of-care conventional imaging. Estimates place annual prevalence of nmCRPC at over 100 000 . It was not until 2018 that next-generation AR antagonists were approved for this indication prior to this time, median bone-related metastasis-free survival was 25 to 30 months . Understanding of this clinical state may evolve as more sensitive imaging techniques such as molecularly-targeted positron emission tomography and whole-body diffusion-weighted magnetic resonance imaging become widely available in clinical practice and are able to detect metastases not previously detected by conventional imaging . Several studies of these advanced imaging modalities detect metastases not seen on conventional techniques .
Hormone Therapy Can Cause Side Effects
Because hormone therapy blocks your bodys ability to produce hormones or interferes with how hormones behave, it can cause unwanted side effects. The side effects you have will depend on the type of hormone therapy you receive and how your body responds to it. People respond differently to the same treatment, so not everyone gets the same side effects. Some side effects also differ if you are a man or a woman.
Some common side effects for men who receive hormone therapy for prostate cancer include:
Recommended Reading: Can Dogs Be Given Melatonin
Treating Prostate Cancer With Combined Hormonal
Androgens, the family of male sex hormones that includes testosterone, function as a fuel for growth in normal development. However, in some men they can also drive the progression of prostate cancer. Hormonal therapy treats prostate cancer by dramatically reducing levels of testosterone and other androgens.
Hormonal therapy is sometimes given in conjunction with external beam radiation to boost the effectiveness of treatment. Hormonal therapy may also be used to shrink the size of large prostate glands before brachytherapy takes place, to enable proper placement of the radioactive seeds.
Combination hormonal/radiation therapy is now a standard option for men with cancer that has extended beyond the prostate or whose cancer is considered high-risk based on other clinical findings, with studies showing that it reduces the risk of dying from prostate cancer and other causes more than with either treatment given alone..
Combination therapy can also be considered for men with localized prostate cancer in the intermediate-risk category. Whether men with low-risk prostate cancer would benefit from a hormonal therapyradiation combination is uncertain.
Image: sturti/Getty Images
What Will I Learn By Reading This
You and your doctor may be talking about using hormone therapy to control your prostate cancer. It is important for you to learn about hormone therapy so that you will know what to expect and how best to take care of yourself before, during, and after treatment. You will learn:
It is important to think about how you will work these things into your everyday life if you and your doctor decide that hormone therapy is the best way for you to control your prostate cancer..
You May Like: What Is Testosterone In Men