Screening For Breast Cancer
Regular mammography examinations to detect early breast cancer have become a key component of national breast cancer screening programmes. Mammography is also required for balanced diagnostic surveillance in epidemiological studies and clinical trials that evaluate the effect of hormones on breast cancer incidence. Menopausal estrogenprogestogen hormones increase the density of breast tissue and may affect the accuracy of mammography interpretation . It is therefore sensible to assess the overall results of breast cancer screening programmes to evaluate whether hormonal effects might cause a significant change in their effectiveness.
The case for breast cancer screening is based on the results of trials: the New York Health Insurance Plan trials and four Swedish trials were the principal randomized trials. Combined results of the Swedish trials in particular show a 27% reduction in mortality from breast cancer in women aged 6069 years invited for screening but failed to show a significant advantage for women aged 4059 years .
Trials of technique showed advantage to double reading and to the taking of two views at prevalent screening. Otherwise screening in the UK has been based on the single lateral oblique view. A trial of the screening of younger women still awaits final analysis.
Your Race And Ethnicity
White and Black women have the highest risk of developing breast cancer in their lifetime. Asian/Pacific Islander and Hispanic/Latina womens breast cancer rates fall in between two major groupings while American Indian and Alaska Native women are on the lowest end of risk.
While white women are more likely to develop breast cancer than Black women overall, they tend to be diagnosed at an older age . Black women have the highest breast cancer rates among women under age 40. Black women make up a higher percentage of triple-negative breast cancer cases.
What to do: If your race or ethnicity places you at higher risk, make sure you follow all screening recommendations to improve your chances of catching cancer early.
Breast Cancer Rates Fell When Regular Hormone Therapy Decreased
Breast cancer rates dropped by half in tandem with the discontinuation of hormone replacement therapy, according to a study published online in the Journal of the National Cancer Institute. The study was reported in the Telegraph in the United Kingdom.
The Telegraph said:
Dr Prithwish De, of the Canadian Cancer Society, and colleagues, found that use of HRT dropped from 12.7 per cent in 2002 to 4.9 per cent in 2004.
During the same period breast cancer rates dropped by 9.6 per cent even though the same number of women were having mammography tests.
Between 2004 and 2006 use of HRT remained stable at around five per cent of women aged 50 to 59 but breast cancer rates began to increase again.
Dr De wrote: The results support the hypothesised link between the use of hormone replacement therapy and invasive breast cancer incidence and indicate that the sharp decline in breast cancer incidence in 2002 is likely explained by the concurrent decline in the use of hormone replacement therapy among Canadian women.
The studys authors said these numbers support existing evidence of the link between HRT and breast cancer.
You May Like: What Is Stage 2 Cancer Of The Breast
Read Also: What’s The Highest Dose Of Melatonin You Can Take
Estrogen Balance For Reduced Breast Cancer Risk
Theres a strong association between estrogen and breast cancer. While there are no guarantees when it comes to cancer, keeping your estrogen balanced through smart lifestyle changes like those Ive listed above can reduce your risk and benefit your overall hormone health.
If you’re looking for a comprehensive approach that can help you achieve optimal hormonal balance, my free Hormone Starter Kit includes a 7 day meal plan, recipes, and other helpful info to get you on the right track.
Are There Any Scientifically Proven Advantages For Rbhrt Over Conventional Hrt
Tolerance
Progestogens may not be alike with regard to potential adverse metabolic effects or associated breast cancer risk when combined with long-term estrogen therapy. Micronised progesterone and some progestogens have specific beneficial effects that could justify their use besides their expected actions on the endometrium. Synthetic analogues of progesterone bind to the glucocorticoid, mineralocorticoid and androgen receptors. This can lead to unwanted side effects such as fluid retention, acne and weight gain. Progestogens and progesterone can lower mood through stimulation of the neurotransmitter gamma amino butyric acid whilst progesterone has sedative effects through its intermediate metabolites, progestogens can cause PMS-type side effects including anxiety and irritability.
Venous thromboembolism
It is well recognised that unlike oral estrogen, transdermal estrogen does not appear to increase the risk of VTE. Observational and case control data suggest that the use of certain progestogens e.g. dydrogesterone and micronised progesterone may reduce the increased risk of VTE conferred by oral estrogen, compared to that noted with other synthetic progestogens.
Cardiovascular risks
Endometrial protection
You May Like: How Can You Tell If You Have Low Estrogen
What Is A Hormone Receptor
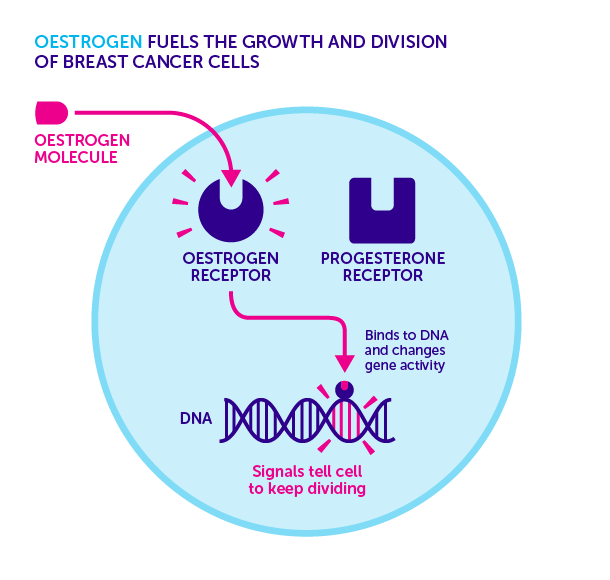
In breast cancer, hormone receptors are the proteins located in and around breast cells. These receptors signal cells both healthy and cancerous to grow. In the case of breast cancer, the hormone receptors tell the cancer cells to grow uncontrollably, and a tumor results.
Hormone receptors can interact with estrogen or progesterone. Estrogen receptors are the most common. This is why ER-positive is the most common form of breast cancer.
Some people are diagnosed with progesterone receptor-positive breast cancer. The key difference is whether cancerous cells are getting growth signals from estrogen or progesterone.
Testing for hormone receptors is important in treating breast cancer. In some cases, there are no hormone receptors present, so hormone therapy isnt a good treatment option. This is called hormone receptor-negative breast cancer.
According to
Recommended Reading: Estradiol Patch Generic Price
How Gene Changes Can Lead To Breast Cancer
Genes control how our cells function. They are made up of a chemical called DNA, which comes from both our parents. DNA affects more than just how we look it also can influence our risk for developing certain diseases, including some kinds of cancer.
Normal cells have genes called proto-oncogenes, which help control when the cells grow, divide to make new cells, or stay alive. If a proto-oncogene is mutated in a certain way, it becomes an oncogene. Cells that have these mutated oncogenes can become cancer.
Normal cells also have genes called tumor suppressor genes, which help control how often normal cells divide in two, repair DNA mistakes, or cause cells to die at the right time. If a cell has a mutated tumor suppressor gene, then the cell can turn into cancer.
Cancers can be caused by gene changes that turn on oncogenes or turn off tumor suppressor genes. Changes in many different genes are usually needed to cause breast cancer.
Also Check: Does Testosterone Cause Hair Loss
How Breast Cancer Forms And Multiplies
Cancer cells are triggered when a mutation in normal cells occur. This can happen due to well-known problematic lifestyle factors like living on junk food, chronic sunburn and cigarette smoking, but hormones can also play a big role. Once cancer cells are born they grow and divide to make more cancer cells, which form a tumor that may contain millions of cancer cells.
Cancers need a blood supply to provide them the oxygen, nutrients and hormones like estrogen, which help them grow and multiply. But as they get bigger they are often further away from the blood vessels so they need to set up their own supply. They do this by sending out signals that tell your body to grow new blood vessels like capillaries. This process is called angiogenesis. And it is ongoing, so once it occurs the cancer keeps getting bigger and then may start to spread to organs like your liver . Thats why scientists are working on cancer vaccines and drugs to try to halt the process of angiogenesis.
Breast cancer is often caused by cancer cells growing in the lobules, where milk is produced or the ducts, where the milk travels to the nipple. Breast cancer cells may then spread to surrounding breast tissue, then move to the lymph nodes under the arms and migrate to other parts of the body.
Read Also: How Likely Am I To Get Breast Cancer
New Research Again Links Increased Breast Cancer Risk To Longer Use Of Hormone Therapy
The link between hormone therapy and breast cancer has been recognized for years. But an analysis published Aug. 29, 2019, in The Lancet has added some additional information to the discussion. The analysis looked at 58 studies that included information on the type and timing of hormone use in individual women, and their body mass index. Researchers began gathering the studies in 1992 and continued until 2018.
We asked Dr. Wendy Chen, an assistant professor of medicine at Harvard Medical School, to help us sort through both the old and new information on hormone use and breast cancer and what it means for women considering starting hormone therapy.
To continue reading this article, you must log in.
- Research health conditions
- Prepare for a doctor’s visit or test
- Find the best treatments and procedures for you
- Explore options for better nutrition and exercise
Recommended Reading: How Do You Test For Testosterone
Prevalence Of Hormonal Steroid Use
Ever use of contraception among women of reproductive age reached 62% worldwide and 70% in the more developed regions in the year 2001 among those who live in a marital or consensual union. Current use of steroidal contraception including oral, injectable and implantable methods exceeded 8% worldwide and 17% in the more developed countries. Current usage rates for steroidal contraception were as high as 48% in The Netherlands, 46% , 36% , 26% , 24% , 20% and 16% .
Use of hormone preparations among menopausal and post-menopausal women is less well documented and more uncertain. In 1997 the worldwide acceptance of menopause hormone treatment among women aged 4564 years was estimated to be 12% .
Also Check: Does All Breast Cancer Chemo Cause Hair Loss
What Is The Link Between Estrogen And Uterine Cancer
Uterine, or endometrial, cancer forms in the lining of your uterus. Women are more likely to develop this cancer after menopause.
Your estrogen-related risk may go up with:
- Estrogen replacement therapy: Estrogen eases menopausal symptoms like hot flashes, night sweats and vaginal dryness. But taking estrogen alone increases the risk of uterine cancer. Combination hormone therapy is less likely to cause uterine cancer. If youve had a hysterectomy, you dont have a uterus and cant get uterine cancer.
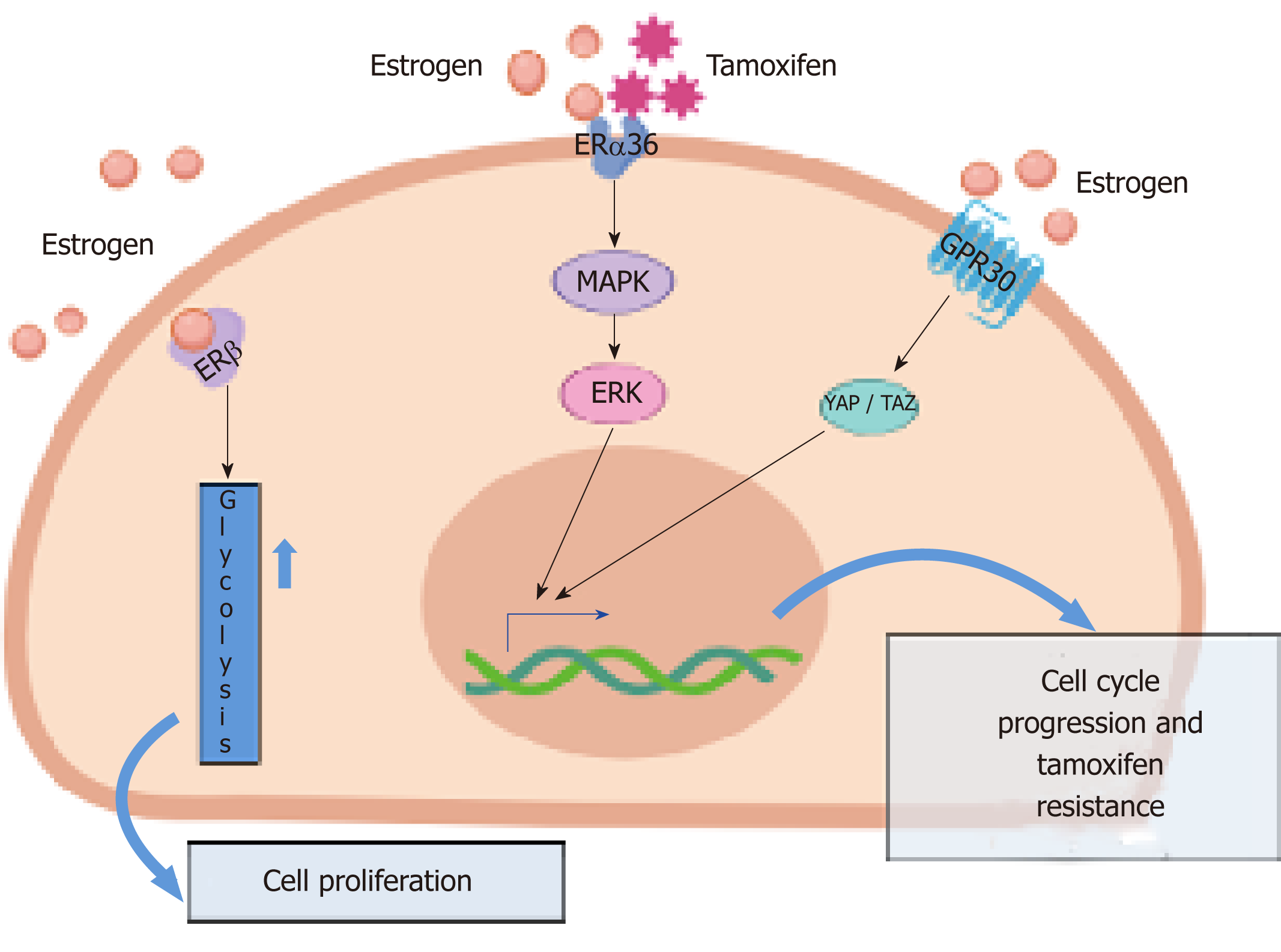
- Tamoxifen: Tamoxifen is a breast cancer drug that lowers the risk of breast cancer and breast cancer recurrence. Its a selective estrogen receptor modulator that blocks estrogens effects on breast tissue. But in menopausal women, tamoxifen acts like estrogen in your uterus. It stimulates the growth of your uterine lining, increasing endometrial cancer risk. Still, the chances of developing endometrial cancer from tamoxifen are less than 1% per year. Theres also a slightly higher risk of uterine sarcoma, a cancer that forms in uterine muscles or tissues.
You May Like: How Long Can I Take Melatonin
Estrogen And Breast Cancer Risk
Estradiol, and possibly estrone, increase the risk of developing breast cancer. And a lower level of these estrogens throughout a woman’s lifetime is associated with a lower risk of developing breast cancer.
Factors such as pregnancy and breastfeeding alter estrogen levels in ways that are believed to have a protective effect. Having a first child before the age of 30, having more children, and breastfeeding are all associated with a lower risk of breast cancer. This is due to the reduced production of estrogens during pregnancy and lactation .
Because some oral contraceptives and hormone therapies contain a combination of estrogen and progestins, they may lead to a slightly increased risk of breast cancer for women.
While it is known that estrogen receptor-positive breast cancers are worsened by estrogen, other breast cancer types typically are also more common among women who have had a higher lifetime exposure to estrogen.
Can You Reduce Your Risk Of Breast Cancer Related To Estrogen
The connection between estrogen and breast cancer is clear, so optimal levels are vital. I wish I could tell you exactly what to do to avoid a breast cancer diagnosis altogether, but of course, I cant because it’s an issue that’s too complex to offer that type of advice.
That said, there are things you can do to keep your estrogen in check:
Remember that estrogen helps us feel healthy and sexy. The key is maintaining balance with other hormones. Here are my top lifestyle habits that promote healthy estrogen metabolism.
- Maintain a healthy body weight. Remember that your fat tissue can make estrogen by converting androgens into estrogens. This means that as body fat increases, so does the amount of estrogen produced and circulated throughout your tissues.
Scientists estimatee that your risk for developing breast cancer jumps by 30% after menopause if your BMI is above 30. And being overweight appears to be linked to ER+ breast cancers, likely related to the increased estrogen production. While its much easier said than done to maintain body weight, the number one tip I advise for healthy weight is a healthy fiber intake. Try swapping your mindset from how many calories did I eat today to how much fiber from real, whole vibrant foods did I enjoy today?
- Keep xenoestrogens out of your kitchen. Chemicals like BPA, phthalates, and BHT all mimic estrogen in the body. They sneak into our kitchen via canned goods, plastic containers, and other food storage items.
Also Check: Anti-mullerian Hormone Test Results
Lowering Estrogen Levels From The Ovaries
This type of treatment only works in premenopausal women who have functioning ovaries. It can help some types of hormone therapy work better. It is also used to treat cancer that has spread.
There are three ways to lower estrogen levels from the ovaries:
- Surgery to remove the ovaries
- Radiation to damage the ovaries so they no longer function, which is permanent
- Drugs such as goserelin and leuprolide that temporarily stop the ovaries from making estrogen
Any of these methods will put a woman into menopause. This causes symptoms of menopause:
- Hot flashes
- Loss of interest in sex
Morning Rounds With Dr Steven Economou At Rush Hospital Breast Cancer Surgeon
Thirty Five years ago, surgeon Steven Economou MD asked me, Does Estrogen cause breast cancer, and does hormone replacement increase cancer recurrence in breast cancer survivors? Back then, I did not know the answer, and neither did he. Thirty Five years later, we now have the answer.
Above left image: Steven Economou MD, Surgeon Rush Medical Center Chicago, courtesy of the NIH and Raphael E Pollock MD , Annals of Surgical Oncology March 2008.
Also Check: What Are The Side Effects Of Bioidentical Hormone Therapy
What Are Hormones And Hormone Receptors
Hormones are substances that function as chemical messengers in the body. They affect the actions of cells and tissues at various locations in the body, often reaching their targets through the bloodstream.
The hormones estrogen and progesterone are produced by the ovaries in premenopausal women and by some other tissues, including fat and skin, in both premenopausal and postmenopausal women and in men. Estrogen promotes the development and maintenance of female sex characteristics and the growth of long bones. Progesterone plays a role in the menstrual cycle and pregnancy.
Estrogen and progesterone also promote the growth of some breast cancers, which are called hormone-sensitive breast cancers. Hormone-sensitive breast cancer cells contain proteins called hormone receptors that become activated when hormones bind to them. The activated receptors cause changes in the expression of specific genes, which can stimulate cell growth.
Breast cancers that lack ERs are called ER negative, and if they lack both ER and PR they may be called HR negative.
Approximately 67%80% of breast cancers in women are ER positive . Approximately 90% of breast cancers in men are ER positive and approximately 80% are PR positive .
Aberrant Hormone Exposure Is More Influential In The Young Rather Than Old Mammary Gland
Aberrant hormone exposures via clinical administration or natural exposure are known to increase the risk of breast cancer. Elevated endogenous hormones increase breast cancer risk dizygotic twins can be exposed to up to two times the maternal estrogen levels that single pregnancies experience . In line with this studies have reported increased breast cancer risk in women later in life who belong to a dizygotic twin pair .
Cumulatively, the epidemiological studies assessing aberrant hormonal exposures again point to the young mammary gland as being the most susceptible to hormone fluctuations and breast cancer risk modulation.
Read Also: Will Birth Control Help Hormonal Acne
Reducing The Cancer Risks Of Hormone Therapy
If you and your doctor decide that MHT is the best way to treat symptoms or problems caused by menopause, keep in mind that it is medicine and like any other medicine its best to use it at the lowest dose needed for as short a time as possible. And just as you would if you were taking another type of medicine, you need to see your doctor regularly. Your doctor can see how well the treatment is working, monitor you for side effects, and let you know what other treatments are available for your symptoms.
All women should report any vaginal bleeding that happens after menopause to their doctors right away it may be a symptom of endometrial cancer. A woman who takes EPT does not have a higher risk of endometrial cancer, but she can still get it.
Women using vaginal cream, rings, or tablets containing only estrogen should talk to their doctors about follow-up and the possible need for progestin treatment.
For women who have had a hysterectomy , a progestin does not need to be a part of hormone therapy because theres no risk of endometrial cancer. Adding a progestin does raise the risk of breast cancer, so ET is a better option for women without a uterus.
Women should follow the American Cancer Society guidelines for cancer early detection, especially those for breast cancer. These guidelines can be found in Breast Cancer Early Detection.