Treatment Side Effects And Complications
Menopause-like symptoms can be difficult for young women being treated for breast cancer. Rather than the gradual onset of natural menopause, hot flashes and other symptoms tend to come on quickly and harshly soon after treatment starts.
Sexual side effects are common with lower estrogen levels, and these can be particularly bothersome for young women as well.
Breast Cancer Doctor Discussion Guide
Get our printable guide for your next doctor’s appointment to help you ask the right questions.
Why Do Some Women Refuse Treatments For Their Breast Cancer
Adjuvant therapy after surgery, such as chemotherapy, hormonal therapy, and radiation therapy, has contributed to a 39% decrease in breast cancer mortality since 1989. Unfortunately, a significant number of women decline evidence-based adjuvant therapy. A recent study suggests that distrust of the medical system plays a significant role in such refusal.
I write about alternative cancer treatments a lot, in particular the lack of evidence for such practices, many of which are at best pseudoscientific and at worst pure mystical nonsense. The reason, of course, is simple. Im a breast cancer surgeon, and I hate seeing people who might be saved from death due to cancer falling prey to treatments that demonstrably lessen their chances of survival, either by leading patients to reject effective treatment in favor of ineffective or even harmful treatments or, at the very least, to delay effective treatment until the patient realizes that the quackery chosen isnt preventing the growth and spread of his or her tumor. This can sometimes take a long time. Ive seen women with breast cancer whose breasts were basically eaten away until there was nothing left but an ulcerated mass on their chestmore than that, a bleeding, rotting, malodorous ulcerated mass. Yes, its an ugly picture, but Ive seen it all too many times.
Side Effects And Risks Of Treatment
Tamoxifen increases the chances of developing endometrial cancer and blood clots in the legs and lungs. In a Danish study, the 5-year risk of developing blood clots was about 1.2% in breast cancer patients taking tamoxifen compared to 0.5% in breast cancer patients who were not taking tamoxifen. Tamoxifen often causes side effects similar to those experienced in menopause, including hot flashes and irregular periods. In one study, 41% of women taking tamoxifen experienced hot flashes, and 10% experienced abnormal periods .
Recommended Reading: Does Melatonin Help With Deep Sleep
Ovarian Suppression In Addition To Chemotherapy
With the known advantages of both chemotherapy and OA/OS alone as monotherapies, additional studies were designed to evaluate the benefit of adding OA/OS to standard chemotherapeutic regimens as well as the reverse scenario of assessing the benefit of chemotherapy when added to OS/OA . In aggregate, these studies do not show a clear overall survival benefit with the addition of OS/OA to chemotherapy, although a small benefit appears to emerge, particularly in younger women with hormone-responsive disease.
The Gruppo Oncologico Centro-Sud-Isole conducted the MAM1 trial with two objectives, to evaluate the addition of doxorubicin to CMF as compared to CMF alone, and to assess the benefit of adding tamoxifen and goserelin to chemotherapy in premenopausal women.24 Of the 466 patients enrolled 79% were ER+ or unknown and the median number of involved lymph nodes was 3. This study showed a significant improvement with the addition of the anthracycline to CMF for DFS , but not overall survival . There was a significant improvement in DFS but not in overall survival , favoring the addition of combined endocrine therapy to chemotherapy. Although the study was not powered to detect differences between the four treatment arms, there was a trend favoring the arm that contained the anthracycline, CMF, and goserelin/tamoxifen .
What Is Hormone Therapy
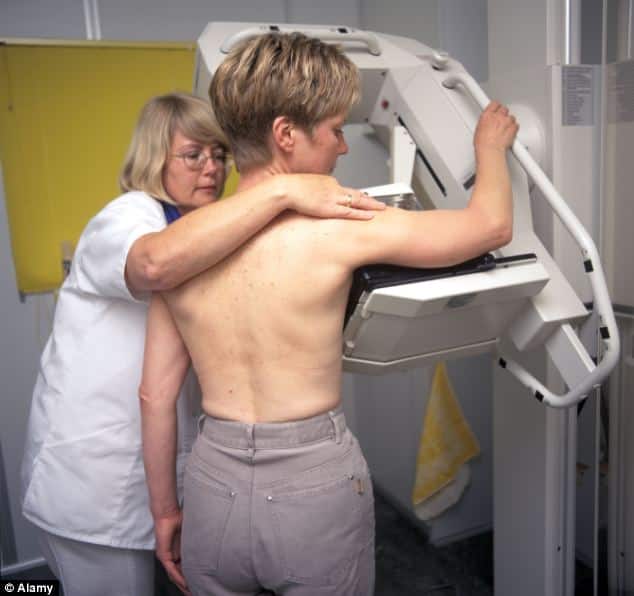
Hormone therapy slows or stops the growth of hormone-sensitive tumors by blocking the bodys ability to produce hormones or by interfering with effects of hormones on breast cancer cells. Tumors that are hormone insensitive do not have hormone receptors and do not respond to hormone therapy.
Hormone therapy for breast cancer should not be confused with menopausal hormone therapy treatment with estrogen alone or in combination with progesterone to help relieve symptoms of menopause. These two types of therapy produce opposite effects: hormone therapy for breast cancer blocks the growth of HR-positive breast cancer, whereas MHT can stimulate the growth of HR-positive breast cancer. For this reason, when a woman taking MHT is diagnosed with HR-positive breast cancer she is usually asked to stop that therapy.
Recommended Reading: Anthem Blue Cross Hormone Replacement Therapy
How Might Extended Therapy Be Applied To Premenopausal Women
As seen in Table 1, fewer than 10% of patients in ATLAS were premenopausal at the time of randomization, which limits generalizations. However, there is a suggestion of a greater absolute reduction in recurrence rate with extended tamoxifen therapy in premenopausal women as compared to postmenopausal women 4. In the NSABP B-14 study described above, analysis conducted by age failed to demonstrate a difference in DFS between groups25.
At present there are no validated assays available to estimate benefit from extended endocrine therapy. Recent data suggest that the Breast Cancer Index, an 11-gene assay that combines Molecular Grade Index to assess tumor grade and proliferation, the HOXB13/IL17BR index, and 4 reference genes, may be helpful for predicting risk of late recurrence, but this tool is not yet recommended for routine clinical use28. Development of such a tool could optimize treatment-decision making, and lead to use of extended treatment in those patients at increased risk of delayed recurrence and to avoidance of treatment and its associated toxicity for those with minimal risk. Current guidelines recommend that patients who remain premenopausal or perimenopausal following five years of adjuvant tamoxifen should be offered extended therapy up to 10 years13,21,29.
Chemotherapy Plus Tamoxifen Vs Chemotherapy Alone
Seven major randomized trials have evaluated the effect of adding tamoxifen to chemotherapy as compared to chemotherapy alone .40â46 These trials are summarized in Table 3. The chemotherapy regimens used and the duration of tamoxifen varied considerably amongst the trials. The EBCTCG meta-analyses did reveal a benefit with adding tamoxifen to chemotherapy in women < 50 with a hazard ratio of 0.65 when they were given concurrently. There was a trend towards reduction in the risk of recurrence when chemotherapy and tamoxifen were given sequentially but the confidence interval was wide. This benefit of adding tamoxifen to chemotherapy was irrespective of age in the meta-analysis with women < 40 deriving similar benefit to older women. Nodal status did not affect the benefit of chemotherapy as node-negative and node-positive women benefited similarly. The effect of adding chemotherapy to tamoxifen resulted in improvements in the risks of recurrence and mortality in ER+ women < 50 as well. The large majority of these studies reflected in the meta-analyses used CMF-based chemotherapy regimens, although anthracycline-containing regimens resulted in similar reductions in recurrence and death.13
You May Like: How To Get Your Hormones Checked
Hormone Therapy For Postmenopausal Women
After menopause, hormone therapy for women with metastatic breast cancer can be an aromatase inhibitor, tamoxifen, fulvestrant or other hormone therapy drug.
If the first hormone therapy stops working and the cancer starts to grow again, a second hormone therapy can be used. If the second drug stops working, another can be tried.
Ovarian suppression isnt helpful for postmenopausal women because their ovaries have already stopped producing large amounts of estrogen.
Learn more about tamoxifen.
Learn more about aromatase inhibitors.
What Is Menopausal Hormone Therapy
Menopausal hormone therapy also called postmenopausal hormone therapy and hormone replacement therapyis a treatment that doctors may recommend to relieve common symptoms of menopause and to address long-term biological changes, such as bone loss, that result from declining levels of the natural hormonesestrogen and progesterone in a womans body during and after menopause.
MHT usually involves treatment with estrogen alone or estrogen plus progestin, a synthetic hormone whose effects are similar to those of progesterone.
Women who have a uterusthat is, who have not had a hysterectomyare generally prescribed estrogen plus progestin for MHT. This is because estrogen alone is associated with an increased risk of endometrial cancer, but estrogen plus progestin is not. Estrogen is used alone only in women who have had a hysterectomy.
Don’t Miss: Does Hormonal Imbalance Cause Hair Loss
Ovarian Ablation Or Suppression
Two basic strategies exist to abrogate ovarian function. Ovarian suppression refers to the use of temporary means to suppress ovarian function, generally with LHRH analogues, whereas ovarian ablationa refers to permanent strategies using either oophorectomy or ovarian radiation. The latter is used rarely in the United States, however, due to concerns about efficacy of this approach.2â4 It should be noted that adjuvant chemotherapy can function indirectly as a form of OS or OA depending on the patient, the type of chemotherapy, and the duration of chemotherapy.
Ovarian ablation via oophorectomy is one of the oldest recorded treatments for breast cancer5 and remains an excellent strategy to eliminate ovarian estrogen production. Before the advent of newer, less invasive surgical techniques, perioperative mortality was up to 5% in women with metastatic breast cancer,6 although currently the operative risk is minimal. Surgical oophorectomy is irreversible as are the subsequent consequences of menopause, such as infertility and increased risk of osteoporosis and coronary artery disease. Potential benefits of this approach include the reduction of the risk of ovarian cancer in women who may be at increased risk for ovarian cancer as well as the cost savings over LHRH agonists for any length of time.
Radiation May Be Better Than Anti
Researchers may have identified a treatment alternative for older women with low-risk forms of breast cancer. It could offer fewer adverse side effects than anti-hormonal drug therapies.
The study found slightly higher survival rates for women over 70 with hormone receptor-positive breast cancer and took anti-estrogen medications than those who were treated with a short dose of radiation. All of the patients had undergone a lumpectomy before these treatments, according to a new report published Monday in the International Journal of Radiation Oncology.
Radiation therapy costs $3,800 or more than anti-hormonal therapy over the average patient’s lifetime, the report found.
Still, researchers suggested radiation therapy could be a good alternative to anti-estrogen medications for some women because it could improve their quality of life without higher mortality risks.
“The reality is anti-hormone therapy is not easy to take long-term and doesn’t offer significantly greater benefits. It can dramatically impact quality of life.” said Dr. Frank Vicini, the report’s co-author and principal investigator at 21st Century Oncology, a Florida-based cancer care services operator of 165 centers across 15 states.
Anti-estrogen treatment may be necessary for five to ten years, according to current recommendations. Vicini said as many as 50% of patients who start anti-estrogen treatment had difficulty managing the side effects and end up stopping the treatment during that time.
Don’t Miss: Hormone Pills For Hot Flashes
Possible Side Effects Of Ais
The most common side effects of AIs are:
- Bone and joint pain
AIs tend to have side effects different from tamoxifen. They don’t cause uterine cancers and very rarely cause blood clots. They can, however, cause muscle pain and joint stiffness and/or pain. The joint pain may be similar to a feeling of having arthritis in many different joints at one time. Options for treating this side effect include, stopping the AI and then switching to a different AI, taking a medicine called duloxetine , or routine exercise with nonsteroidal anti-inflammatory drugs . But the muscle and joint pain has led some women to stop treatment. If this happens, most doctors recommend using tamoxifen to complete 5 to 10 years of hormone treatment.
Because AIs drastically lower the estrogen level in women after menopause, they can also cause bone thinning, sometimes leading to osteoporosis and even fractures. If you are taking an AI, your bone density may be tested regularly and you may also be given bisphosphonates or denosumab , to strengthen your bones.
Less Common Types Of Hormone Therapy
Some other types of hormone therapy that were used more often in the past, but are rarely given now include:
- Megestrol acetate , a progesterone-like drug
- Androgens , like testosterone
These might be options if other forms of hormone therapy are no longer working, but they can often cause side effects.
Also Check: Does Spironolactone Help With Hormonal Acne
Risk Of Late Relapse In Hr+ Breast Cancer
The risk of relapse in breast cancer varies over time and is dependent on a number of prognostic features including stage, histopathology, and HR status. Distinct from HR-negative breast cancer that typically has the highest relapse rates early after diagnosis, HR+ breast cancer has a unique predilection for late relapses23. Based on Surveillance, Epidemiology, and End Results data, HR+ breast cancer has an estimated annual hazard rate for relapse of approximately 12% that plateaus and persists through years 101524.
Classes Of Hormone Therapy
Anti-Estrogens
An antiestrogen or estrogen blocker works by blocking estrogen receptors in breast tissue. While estrogen may not cause breast cancer, it is needed for the cancer to grow in some breast cancers. With estrogen blocked, the cancer cells that feed off estrogen may not be able to survive.
|
Generic Name |
|---|
|
Estrogen receptor antagonist |
Side Effects
Every person reacts differently to medications, so it is hard to predict what side effects each patient will have. However, the most common side effects in this category of medications include hot flashes, night sweats, weight gain, vaginal dryness and nausea. Blood clots and endometrial cancers are rare but can occur with these medications.
Aromatase Inhibitors
In women who have gone through menopause, estrogen is mainly made by converting androgens into estrogens. An enzyme called aromatase makes this conversion happen. Aromatase inhibitors block this conversion, leading to less estrogen in the body.
|
Generic Name |
|---|
|
Lupron® |
LHRH agonist, works by stopping production of leutinizing hormone by the pituitary gland. LH causes the ovaries to make estrogen. |
Anti-Androgens
|
Generic Name |
|---|
Also Check: How To Test For Hormone Imbalance
Hormone Therapy For Premenopausal Women
For premenopausal women with metastatic breast cancer, hormone therapy almost always begins with ovarian suppression and either an aromatase inhibitor, tamoxifen or other hormone therapy drug.
Ovarian suppression lowers hormone levels in the body so the tumor cant get the estrogen it needs to grow. This may involve surgery to remove the ovaries or, more often, drugs to stop the ovaries from producing hormones.
Combining ovarian suppression and a hormone therapy drug improves survival over either treatment alone .
If breast cancer progressed during past treatment with a hormone therapy drug, the same hormone therapy drug may not be an option for treatment.
Learn more about ovarian suppression.
Learn more about tamoxifen.
Learn more about aromatase inhibitors.
How Do The Hormones Used In Mht Differ From The Hormones Produced By A Womans Body
The hormones used in MHT come from a variety of plants and animals, or they can be made in a laboratory. The chemical structure of these hormones is similar, although usually not identical, to those of hormones produced by womens bodies.
Non-FDA-approved hormone products, sometimes referred to as bio-identical hormones, are widely promoted and sold without a prescription on the Internet. Claims that these products are safer or more natural than FDA-approved hormonal products are not supported by credible scientific evidence. The FDA provides more information about these products on its Menopause page.
You May Like: Over The Counter Male To Female Hormones
Findings Could Help Improve Treatment Decisions
- Date:
- Washington University School of Medicine
- Summary:
- Hormone therapy can be very effective for so-called estrogen receptor-positive breast cancer. But it only works for a little more than half of women who receive the treatment. In a small study, researchers found that women whose tumors did not respond to a one-day estrogen challenge did not benefit from hormone therapy. The findings could help doctors choose treatments most likely to help their patients.
Hormone therapy commonly is given as a targeted treatment for women whose cancer cells carry receptors for estrogen. But the therapy only works for about half of all patients. Until now, there hasn’t been a good way to reliably predict who will benefit and who will not.
Researchers at Washington University School of Medicine in St. Louis have shown they can distinguish patients likely or unlikely to benefit from hormone therapy using an imaging test that measures the function of the estrogen receptors in their cancer cells. In a small phase 2 clinical trial, the researchers showed that the cancers of all patients with working estrogen receptors remained stable or improved on hormone therapy, and progressed in all women with nonfunctional estrogen receptors. The findings, published Feb. 2 in Nature Communications, could help doctors choose among treatment options and reduce the chances that women would receive a therapy unlikely to help.
Story Source:
Journal Reference:
Cite This Page:
Aromatase Inhibitors Such As Arimidex Femara And Aromasin
Aromatase inhibitors work by blocking the production of estrogen in the body. They are generally reserved for postmenopausal women with breast cancer whose estrogen is primarily produced by the aromatase enzyme. Aromatase inhibitors may be used in premenopausal women if ovarian suppression treatments are also used.
Unlike tamoxifen, aromatase inhibitors have a low risk of causing uterine cancer or blood clots. However, aromatase inhibitors can cause muscle and joint pain, which can lead to some women discontinuing treatment. Because they block the production of estrogen, aromatase inhibitors can cause bone loss in women after menopause.
Common side effects of aromatase inhibitors include vaginal dryness, muscle pain, joint aches, and hot flashes or night sweats.
Recommended Reading: Can You Give Dogs Melatonin Gummies